Overview
At the Center for Thoracic Cancers, our multidisciplinary team of lung cancer specialists put together a comprehensive treatment plan just for you. Many lung patients benefit from our approach. You will see lung cancer specialists from medical oncology, radiation oncology and surgery. We:
- Offer a collaborative approach to lung cancer diagnosis and treatment
- Provide care and support tailored to each patient’s needs
- Combine clinical expertise, cutting-edge research and medical technologies to offer patients the most appropriate therapies
- Ensure patients fully understand their diagnosis and treatment options
- View patients and their family and friends involved in their care as team members
Patients are seen within one week of referral. Urgent within 1-2 days.
Innovative Approaches
The Center for Thoracic Cancers is among the first in the nation to provide new targeted therapies for non-small cell lung cancer. Consistently ranked as one of the best in the country by U.S. News & World Report, we provide promising new therapies and innovative approaches to clinical care, including:
- Expertise in minimally invasive surgery for lung cancer, including lung-sparing techniques
- Genotyping (molecular fingerprinting) to determine which lung cancers carry genetic mutations that might be treated with targeted therapies
- Rapid diagnosis and staging of all biopsied tumors by pathologists who specialize in lung cancer
- Groundbreaking research regarding the molecular basis of some lung cancers
- Access to Proton Therapy at New England’s only proton radiation facility
- Access to one of New England’s only Advanced Endoscopy Services
Lung Cancer Treatment
Learn about the signs, symptoms and causes of lung cancer
Expertise in Diagnosing and Staging Lung Cancer
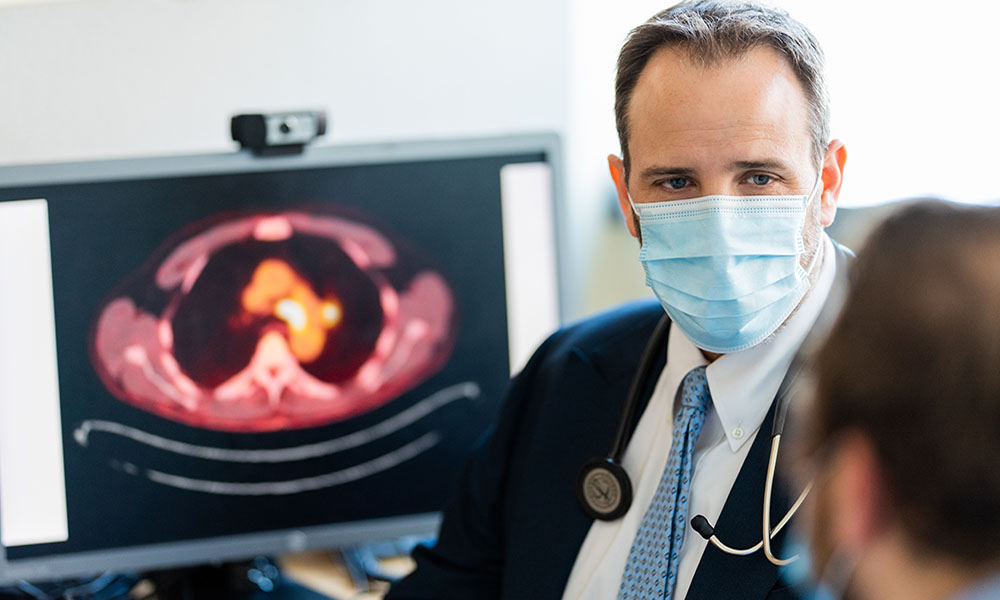
All members of our team of pathologists and radiologists are nationally recognized for their expertise. Our pathologists participate in weekly tumor board meetings, sharing information about each patient’s unique cancer with the entire team to help guide care planning. Our radiologists use the most advanced imaging tools to diagnose and stage thoracic cancers and to detect changes in tumors. Our imaging methods include:
- Chest radiograph
- Computed tomography scan (CT or CAT scan)
- MRI
- PET and nuclear medicine scans
Our minimally invasive image-guided procedures for diagnosis include:
- Percutaneous needle biopsy and molecular diagnostic tests
- Esophageal ultrasound
- Navigation bronchoscopy for biopsy of peripheral lung nodules
Cancer Early Detection and Diagnostics Clinic
The Cancer Early Detection and Diagnostics Clinic at Mass General Cancer Center provides patients with comprehensive cancer diagnosis in one location, bridging the gap between clinical care and research in cancer early detection.
Excellence in Surgical Care
Our team of dedicated surgeons treats some of the most challenging and complex cases from across the US. We focus only on thoracic surgery and have pioneered many now-standard procedures used to treat thoracic cancers. The team provides state-of-the-art evaluation, treatment and post-surgical services, including:
- Chest and airway reconstruction
- Laser surgery
- Minimally invasive video-assisted thorascopic surgery
- Resection of tumors in the chest wall, lungs and mediastinum
- Lung-sparing techniques for benign and malignant neoplasms of the lung
- Resection of tumors obstructing a bronchus or in the trachea
We offer many minimally invasive surgical procedures, such as:
- Bronchoscopy to explore the bronchial passages
- Navigation bronchoscopy to biopsy peripheral lung nodules or placement of radiosurgical markers to enhance tracking of the lung tumors during radiation treatment
- Esophagoscopy to sample lymph nodes around the airway or lung
- Mediastinoscopy to explore the area between the lungs and nearby lymph nodes
- Thoracoscopy to explore the thorax
- Esophageal endoscopic ultrasound
- Endobronchial ultrasound
Learn more about Mass General's Lung Cancer Surgery Program.
Pioneering Radiation Therapy Programs
Specialists in the Thoracic Radiation Oncology Program employ high-precision radiation therapy to treat patients with lung cancers and other cancers in the chest with the overarching goal of causing little or no side effects. Pioneering technological advances for the benefit of our patients include:
- Intensity-modulated radiation therapy (IMRT) and Volumetric Modulated Arc Therapy (VMAT) for reducing side effects and improving tumor kill
- Stereotactic Body Radiation Therapy (SBRT) for the treatment of early stage lung cancers and increasingly also metastatic cancers
- 4-dimensional (4D) CT scanning and respiratory gating for treatment of lung tumors that move around with breathing
- Proton therapy in patients with certain lung cancers
Our radiation oncologists are part of a highly specialized multidisciplinary team that closely coordinates the care of each patient. Cutting-edge research aims at increasing the efficacy and reducing the side effects of radiation therapy as well as integrating radiation with revolutionizing biological drug therapies.
For more information, please see the Thoracic Radiation Oncology Program.
Lung Cancer Clinical Trials
Clinical trials are research studies which are conducted to answer questions. They can test many things including new drugs, new combinations of drugs, or already approved drugs being studied to treat patients in new or different ways. They may include new drug doses or new ways (schedules) to give the drugs. Clinical trials are run under strict guidelines with specific criteria for eligibility and treatment. Their purpose is to help find out whether new cancer treatments are safe and effective or better than the standard (current) treatment.
Our program has a very active clinical research portfolio with the latest, top-notch investigational studies covering a wide spectrum of thoracic cancer care. The ultimate goal of clinical research is to improve the outcomes for all of our patients. If you are eligible for a clinical trial, your physician will offer you the chance for participation. We will comprehensively review the logistics and purpose of the trial and also offer alternatives including the standard of care.
Find Clinical Trials for Lung Cancer.