Every Second Matters for Emergency and Essential Surgery – Ketamine (ESM-Ketamine)
Millions of people are not able to access basic surgical care, particularly emergency cesarean section and other reproductive health procedures, due to a lack of anesthesia services. To address this gap and through the support of a Saving Lives at Birth Grant (USAID, the Government of Norway, the Bill & Melinda Gates Foundation, Grand Challenges Canada, DFID, and KOICA), Mass General is working with Sagam Community Hospital to implement a best-evidence package, Every Second Matters for Mothers and Babies - Ketamine for Painful Procedures and Emergency Cesarean Section (ESM-Ketamine).
As of July 30, 2019, 1,965 lives have been saved and/or improved through the implementation of the ESM-Ketamine package.
The Challenge
The lack of anesthesia services is a well described crisis in resource constrained settings worldwide. The consequences of this gap are that millions of women are unable to access emergency cesarean section and other critical reproductive health procedures. The burden of disease and disability resulting from a lack of anesthesia services has never been quantified or reported in the literature, but is unquestionably staggering. A recent Kenya Ministry of Health (2011) study of the Nyanza region identified that for a population of 5.8 million people, there are 34 operating theatres with associated doctors able to perform cesarean section and other basic surgical procedures. However, there are only 18 anesthetists in the region, and 15 of the 34 theatres report absolutely no access to anesthetist services.
The Innovation
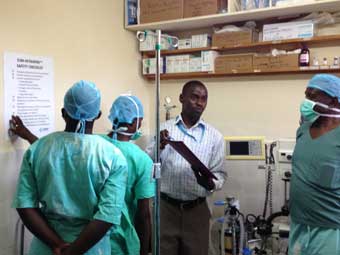
Mass General is working closely with faculty from Sagam Community Hospital and Maseno University Medical School to carefully implement a task shifting, carefully bounded disruptive pilot program at 4 institutions with operating theatres but no anesthetist services: Sagam, Maseno Mission, Coptic, and Yala Sub-District hospitals. The innovation is a best evidence package on the use of ketamine for painful procedures and emergency cesarean section, building on the WHO approach to safe surgery. Ketamine is a unique dissociative agent that has been used worldwide for over 40 years. Ketamine has a long and well reported track record of extraordinary safety and countless unreported anecdotes on safe use by doctors, nurses, and nurses’ aides in Kenya and all across Africa. While virtually all other sedative agents compromise airway and hemodynamic reflexes by their very nature, ketamine enhances minute ventilation and other respiratory and hemodynamic properties. We believe that these unique features allow for a great opportunity to develop and test a carefully controlled task shifting package. During the first week of November 2013, we trained 9 Kenyan health care providers (2 medical officers, 2 clinical officers, 4 nurses, and 1 nurse's aid) at Sagam Community Hospital in a best evidence package, ESM-Ketamine. In the second week of January 2014, we trained 6 additional providers (4 clinical officers and 4 nurses) at Maseno Mission, Coptic, and Yala Sub-District hospitals. The four-day trainings included basic pharmacology, basic monitoring, Helping Babies Breathe, and case-based learning through oral exercises and actual operating theatre time. As part of the ESM-Ketamine package, each of the 4 institutions has been given a standardized ESM-Ketamine kit and wall chart, and each provider a pocket checklist.
Support the Global Health Innovation Laboratory
Your support helps us improve health care and save lives for some of the neediest populations around our globe.
