News5 Minute ReadMay | 1 | 2023
Addressing Capacity in the Neuroscience ICU: NSRU Improves Outcomes for Stroke Patients
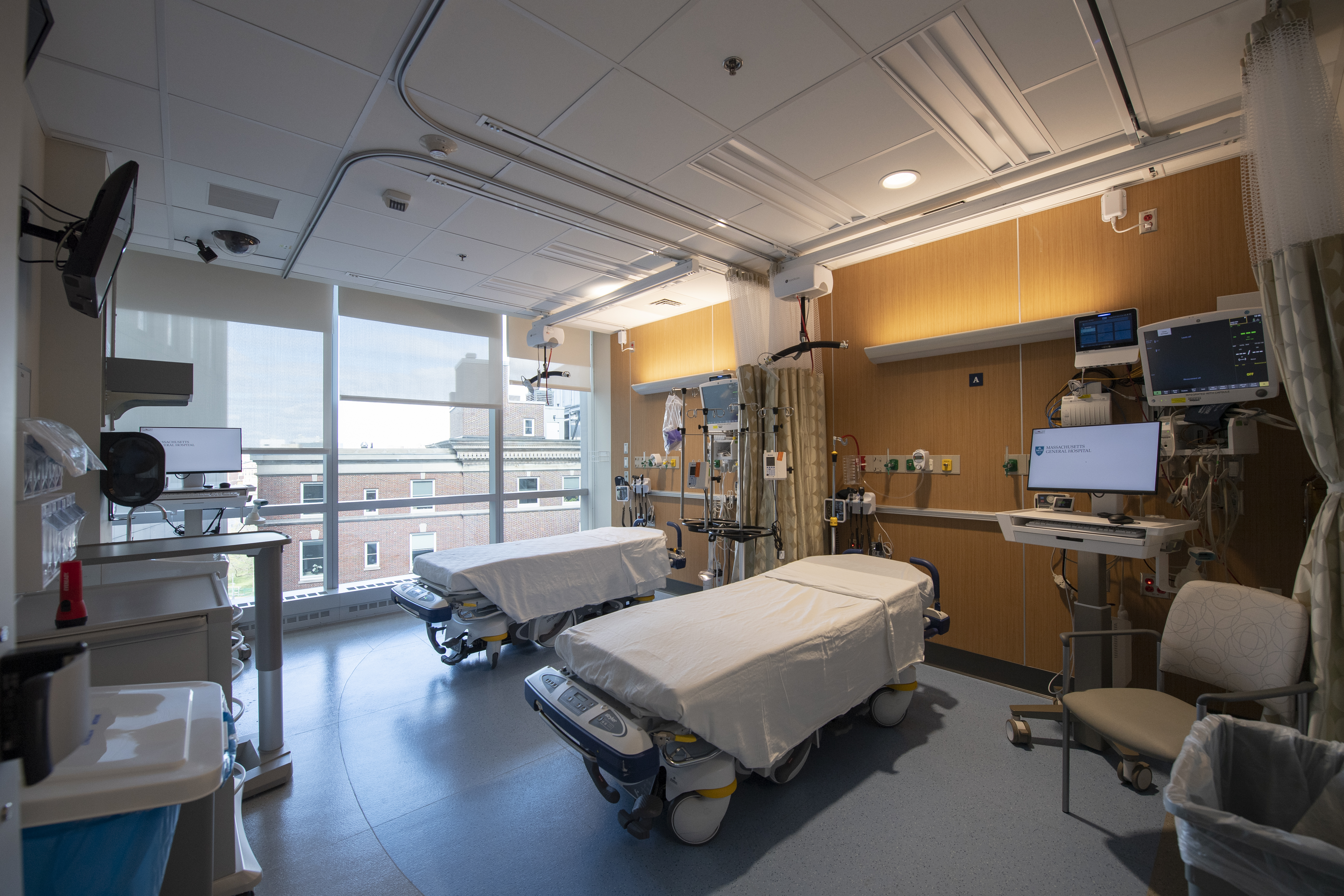

For patients experiencing stroke or other serious brain or nervous system conditions, time is always of the essence.
To deliver this highly specialized, time-sensitive care to patients quickly while also helping to combat ongoing capacity challenges, a multidisciplinary team in the departments of Neurology and Neurosurgery developed the Neurosciences Receiving Unit (NSRU) – a new space that can receive transfer patients in need of urgent care following a stroke, even when a bed is not immediately available in the Neuroscience Intensive Care Unit (ICU). When a transfer request comes in from an outside hospital, the MGH Capacity Coordination Center works with a neurointensivist or neurosurgeon to determine whether the patient would be a candidate for the NSRU.
“The NSRU is essentially a small ‘express’ emergency department within the Neuroscience ICU,” says Bob Carter, MD, chair of Neurosurgery. “Patients in need of immediate, lifesaving neurocritical care can come to MGH knowing their injury or illness will be treated with the highest priority right at the bedside to determine the best treatment course. The goal of the NSRU is to increase capacity while improving patient outcomes.”
The NSRU sits adjacent to the Neuroscience ICU at the Mass General main campus and became fully operational in February 2023. W. Taylor Kimberly, MD, PhD, chief, MGH Division of Neurocritical Care, says there are three types of patients who potentially qualify for treatment in the space – someone who has a sudden neurological deficit due to stroke, subarachnoid hemorrhage or large brain tumor, typically from mass effect or seizure.
“A typical situation would be a patient goes to outside hospital and the ED staff member there gets the scan and discovers this is a life-threatening brain injury. They know that the patient needs high-level, multidisciplinary, tertiary level neuroscience expertise and that they need to get them here fast because if they don’t, the patient could die,” says Kimberly. “When this happens, they call the MGH, and we determine whether the patient qualifies for this low-friction transfer pathway and, if so, we bring them in. The idea behind the unit is that many of these patients will need an emergency intervention or treatment that could be lifesaving.”
Before the NSRU space was created, physicians from outside facilities and emergency departments would often need to make multiple calls before finding an open transfer hospital bed. Aman Patel, MD, director of Stroke Intervention at Mass General, says that, for many patients, faster intervention means better recovery. The goal of the NSRU is to increase the speed by which a patient can get that lifesaving care – a patient arriving on the unit can begin necessary testing and imaging right away as it is staffed 24 hours a day, 7 days a week and leverages the expertise of the entire neurocritical care team.
“As soon as we get the call that a patient needs or could potentially need treatment in the NSRU, we evaluate the situation and often get them to the MGH immediately,” says Stephanie Qualls, RN, nursing director, Neuroscience ICU. “We work behind-the-scenes to get the patient here efficiently and quickly and facilitate the next steps in treatment immediately upon arrival.”
Qualls expects NSRU volume to increase as other hospitals – within Mass General Brigham as well as other area hospitals – realize they can send appropriate candidates to Mass General right away.
“When we’re able to get patients into the operating room quickly, they are more likely to get return of function and go back to leading a life with minimal or no disability,” she says.
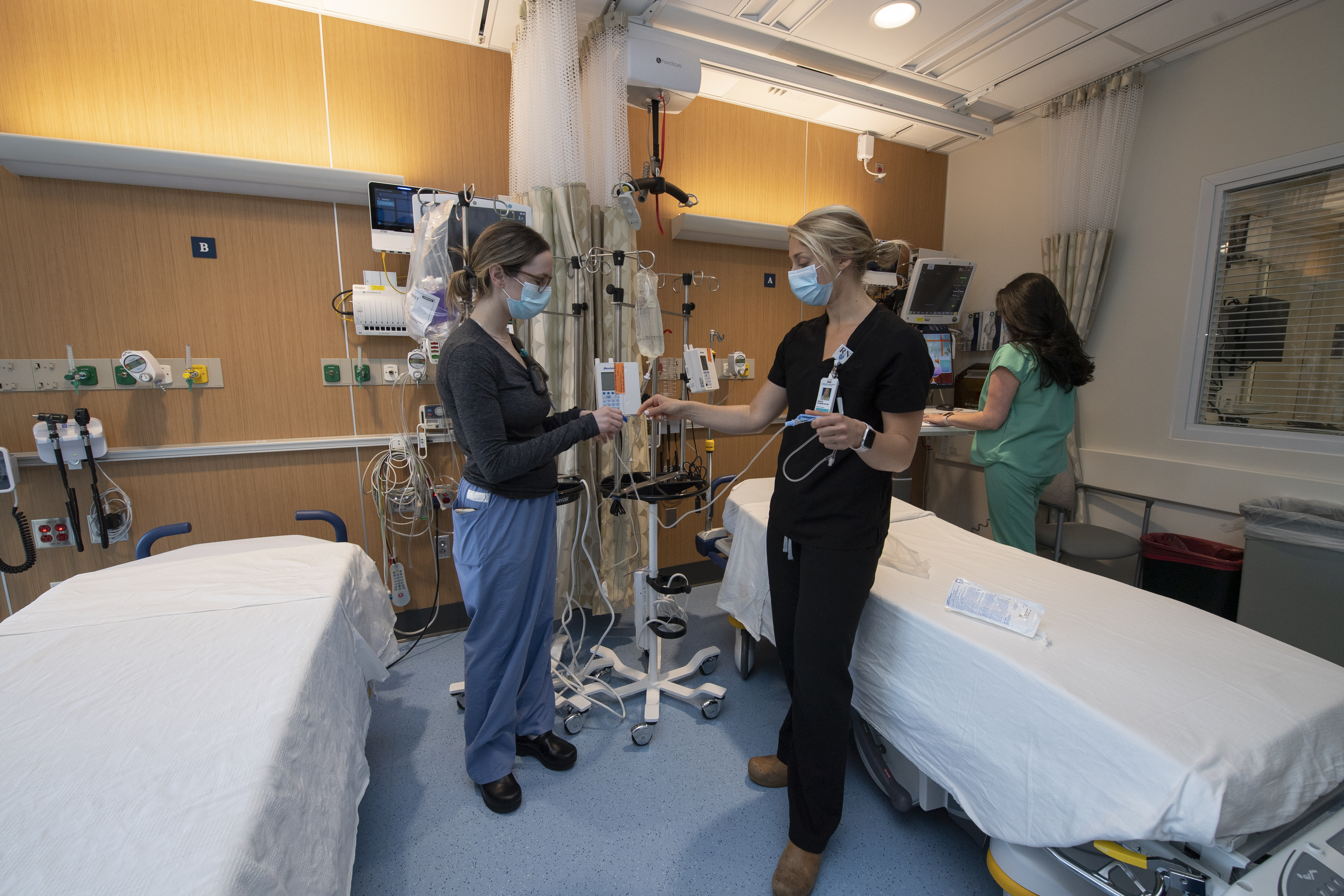 In addition to improving outcomes for patients, the NSRU has been rewarding for staff, too. By nature, it is a highly collaborative space, and patients often improve significantly during their time on the unit. Nurses on the floor played a large role in designing the room, deciding where equipment would fit best and imagining how it would feel to work in the space. The team met weekly with architects to view blueprints and diagrams and optimize the space. They eventually landed on a layout that will allow for two patients to fit in the room when COVID-19 protocols allow.
In addition to improving outcomes for patients, the NSRU has been rewarding for staff, too. By nature, it is a highly collaborative space, and patients often improve significantly during their time on the unit. Nurses on the floor played a large role in designing the room, deciding where equipment would fit best and imagining how it would feel to work in the space. The team met weekly with architects to view blueprints and diagrams and optimize the space. They eventually landed on a layout that will allow for two patients to fit in the room when COVID-19 protocols allow.
“We spent a great deal of time getting buy-in from nurses, advanced practice providers, our Stroke Team – anyone who would end up caring for patients there,” Qualls says. “It was important for us to do mock run-throughs of what it would be like to receive a patient in that kind of unit and identify any vulnerabilities we needed to work out. We’ve learned a lot from this experience, and it feels good to be taking these additional steps to open up access to more patients in the MGH community.”
