Patient StoryFeb | 12 | 2021
Meg’s story: Tethering surgery helps dancer with scoliosis stand tall once again

In a local theater in Huntsville, Ala., the holiday spirit filled the air as families watched their children perform in the classic Christmas ballet, The Nutcracker. Huddled in the fictional Stahlbaum living room, a mischievous Fritz rallies his friends to steal the dolls that Herr Drosselmeyer had just gifted to his sister, Clara, and her friends. Playing the role of a party boy in Fritz’s devilish entourage, Meg Armstrong, 14, along with her fellow performers, prepared to surprise Clara’s circle of friends.
Dance and musical theater have been Meg’s greatest passions since she was 3—and without a critical surgery to correct her scoliosis, her performance career almost ended prematurely. When she was 8 ½, Meg, of Huntsville, Ala., was diagnosed with moderate early onset scoliosis. Meg began seeing a local orthopaedic surgeon who would monitor her curves. The surgeon then discussed the possibility of Meg wearing a brace and needing spinal fusion later in life if the curves progressed. The curves held steady for a few years before they slowly, but steadily began to increase.
During spinal fusion surgery, an invasive procedure, surgeons connect two or more vertebra with metal rods to keep the spine straight. These rods, however, limit the spine’s natural movement. Later in life, the rods can also wear down the vertebra on either side of the rods. Meg and her mother, Kelly, were hesitant—Meg needed to maintain her flexibility to thrive on stage. Spinal fusion would limit her spine’s natural mobility and possibly her future as a performer and dancer.
When Meg was 10, she started wearing a back brace at night. However, the curves in her spine were still progressing. Typically, curves in scoliosis progress about 1–2° per year. Meg’s curves were progressing about 3–5° per year. In January 2020, Meg’s ballet teacher expressed concern about the shift in Meg’s upper body. Three months prior, in October 2019, Meg had seen her doctor for a check-up on her spine. Kelly was shocked by how much the curves had progressed in such a short time.
One day at a hair salon, Kelly discussed her daughter’s scoliosis with her stylist, who recalled another client with a similar experience. “She had a client whose daughter has scoliosis and had tethering surgery. She was doing great as a competitive cheerleader and she didn’t have any loss of flexibility,” said Kelly. “I’d never heard of it until then. Sometime later, that client and I happened to be in the salon at the same time and we started talking.”
Anterior vertebral tethering surgery, or simply tethering, is a surgical procedure that aims to correct spinal curvature and maintain the spine’s natural growth, function and mobility. In tethering surgery, a doctor places titanium screws and a flexible cord along the outer edge of the spinal curvature. As children grow, the screws and cord gently guide the vertebra into a straighter position.
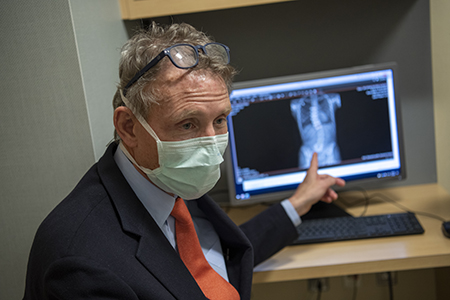
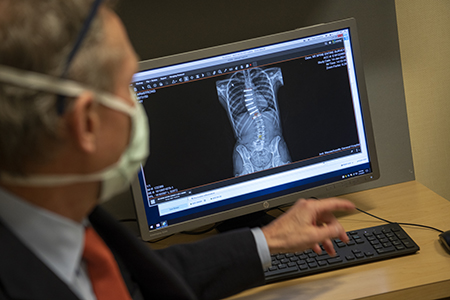
In her search to learn more about tethering, Kelly discovered a Facebook group for parents whose children had this type of surgery. She noticed many parents mentioned a pediatric orthopaedic surgeon named John T. Braun, MD, of Pediatric Orthopaedics and Pediatric Orthopaedic Surgery at MassGeneral for Children (MGfC). Braun performs tethering surgery as a team with Brian Grottkau, MD, chief of the Pediatric Orthopaedic Surgery, and David Lawlor, MD, a pediatric surgeon in Pediatric Surgery at MGfC.
The team approach, said Braun, is the real differentiator. “It improves safety, efficacy and outcomes. Patients and families also appreciate the thoroughness and attention afforded by our unique and consistent team.”
In February 2020, Meg, her father, Stephen, and Kelly flew to Boston for an appointment with Braun. Immediately, they were impressed.

“Dr. Braun is one of the most thorough surgeons I’ve ever met. He was kind, calm and made our experience the least stressful it could have been,” said Kelly. ”Many people haven’t heard of tethering surgery and there are a limited number of surgeons who do the procedure. We were so lucky to find Dr. Braun and his team, knowing Meg would be cared for by a top surgeon at one of the country’s top hospitals.”
Initially, Meg’s surgery was scheduled for April 2020, but had to be rescheduled to June after the COVID-19 pandemic began in March and was seriously affecting the greater Boston area. By the time Meg and Kelly returned, the curves in Meg’s back had progressed even more.
“She had a had a 50° curve in her thoracic spine and a 42° lumbar curve,” said Kelly. “Her shoulder blades were uneven and the shift in her upper body was very noticeable.”
Throughout Meg’s surgery and hospital stay, the Armstrongs felt safe at MGfC despite the ongoing pandemic. From the Child Life Specialists who helped prepare Meg to have an IV placed before going into the operating room, to the surgeons dedicated to Meg’s wellbeing, and the nurses, physical therapists and PCAs who checked on her while she recovered, the Armstrongs called the level of care unmatched.
“Dr. Braun, Dr. Grottkau and Dr. Lawlor are such an excellent team,” said Kelly. “The team approach to this surgery is a benefit to patients and the care they receive at MGfC.”
After surgery, the difference in Meg’s posture and confidence was hard to miss.
“The biggest difference I notice is that my trunk is no longer shifted to one side. I am much happier with my appearance,” said Meg. “I don’t have any pain and my left ribs aren’t sticking out like they used to.”
Kelly and Meg flew home 11 days after surgery. Within 2–3 weeks, Meg was off all pain medications. Within three months, she was ready to return to dance training with all her original flexibility, mobility and grace. In January 2021, Meg began auditioning for summer ballet intensives and hopes to compete in the Youth American Grand Prix, a nonprofit international student ballet competition dedicated to dance education, in 2022.
“Dr. Braun told us once she fully recovers to go ride rollercoasters and forget about scoliosis. Within a week or two, she was feeling good and wanted to know if she could jump on the trampoline. Of course, we said no, she had to wait, but I was happy to see her feeling better,” said Kelly. “In our experience, there is no better place than MGfC to seek care for a child. You are in the best hands possible and hopefully, other families can put scoliosis behind them as well.”
-
![]()
- Orthopaedic Spine Surgeon
- Pediatric Spine & Scoliosis Surgeon
-
![]()
- Pediatric Surgery
- Department of Surgery
Related Pages
Type
Centers and Departments
Spinal Tethering Device Revolutionizes Scoliosis Treatment
Read about spinal tethering for adolescent idiopathic scoliosis, created by John Braun, MD, of Pediatric Orthopaedics and approved by the FDA in 2019.
Tethering Surgery for Scoliosis: What You Need to Know
Tethering surgery helps correct scoliosis in children and teens. Learn about tethering surgery, including what it is and how it helps scoliosis.
Appointments and Referrals
Request an appointment or second opinion, refer a patient, find a doctor or view test results with MGfC's secure online services.



