NewsDec | 21 | 2020
It’s a bird! It’s a plane! It’s a preemie!

Pediatric patients in Mass General for Children’s neonatal intensive care unit (NICU) show strength and determination that can match any superhero. There, infants are treated for a wide variety of medical complications with some spending months in intensive care. Babies born before 32 weeks gestation are particularly vulnerable because their organs are underdeveloped, are unable regulate body temperature and cannot eat or breathe without assistance.
In June, the NICU launched the Small Baby Initiative, a multidisciplinary program that draws on national best practices to improve NICU patient outcomes at Mass General for Children (MGfC) for premature infants born before 23 weeks gestation. Megan Aurora, MD, associate medical director of neonatology, Margaret Settle, RN, PhD, NE-BC, NICU nursing director, Carolyn Bleiler, RN, nursing practice specialist and Carolyn LaVita, MHA, RRT, associate director of Respiratory Care Services, tapped several specialties, including pharmacy, nursing, occupational therapy and nutrition services to study, to evaluate and improve current treatment protocols that are expertly designed for the tiniest of patients.
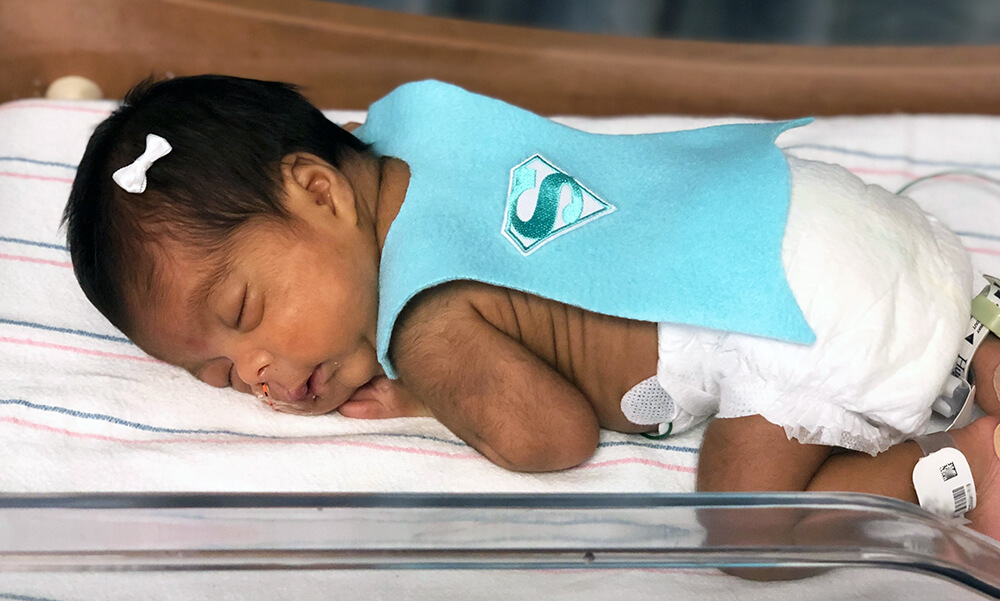
These “small but mighty” babies begin their NICU journeys by donning superhero teal capes that then visually celebrate their growth milestones like weight gain and graduation from incubators from admission to discharge for both physicians and families. “They are our superheroes too and are putting in the hard work to grow. We’re fighting for them, but they’re fighting for themselves,” says Aurora.
The initiative’s goal is to improve clinical care, define hospital best practices and become an international leader in neonatal medicine. Its first phase on improving respiratory outcomes in small babies and cases of bronchopulmonary dysplasia (BPD), a common breathing disorder in infants that can cause lifelong respiratory issues, in part thanks to use of a new device called the bubble CPAP. The machine uses a combination of oxygen, water, and tubing to provide air pressure to the infants lungs, making easier for them to breathe without a ventilator. Bubble CPAPs use is labor intensive and increases necessary bedside care from nurses and respiratory therapists to make sure the machine is working properly at all times.
“It was a culture change,” says Aurora. “People put in the effort to learn a new skill and double their workload because they knew it was best for our babies.”
Since its creation, the Small Baby Initiative has discharged 13 babies and expects to treat 70 infants each year. Its second phase will focus on partnering with the Department of Obstetrics & Gynecology to improve thermoregulation of babies in the delivery room, a difficult practice many NICUs across the country struggle with.
Aurora says, “When very premature infants are born, it’s usually the last thing their family was expecting, and the experience can be a monsoon of emotions and worry. The good news is neonatology has come a long way and gives these babies a great shot at a good outcome. Our NICU team is dedicated to staying up to date on practices that have gotten us to this exciting moment in neonatal medicine, as well as optimizing positive experiences for families along the way.”
-
![]()
- Associate Medical Director of Neonatology
- Instructor in Pediatrics, Harvard Medical School
Related Programs
Type
Centers and Departments
Topics
Exceptional Pediatric Care
A new model for children's health care: learn more about Mass General Brigham for Children.


