Patient StoryApr | 3 | 2023
An Incidental Finding, Life-Saving Care: Surgery to Remove Lindsey’s Pancreatic Tumor


After a long day of summer camp, Lindsey Scheyer, a normally vivacious and energetic 11-year-old, returned home feeling nauseous and bothered by a jabbing pain in her abdomen. Over the course of the evening, her condition worsened to the point where she was vomiting and unable to stand on her own. Her parents, Mark and Emily, rushed her to the emergency room at Newton-Wellesley Hospital, where she normally received her routine pediatric care.
Lindsey was seen by Peter Masiakos, MD, a pediatric provider at Newton-Wellesley and Mass General for Children, which are both part of the Mass General Brigham health system. Dr. Masiakos ordered an ultrasound which soon confirmed his suspected diagnosis that she was suffering from an inflamed appendix (appendicitis). He scheduled her for surgery the next morning to remove it.
During the appendectomy, Dr. Masiakos discovered that her appendix was much more inflamed than what is typically seen with appendicitis. In combination with lingering pain and a persistently high white blood cell count despite the successful appendectomy, Dr. Masiakos surmised that Lindsey was suffering from an infection and recommended that she undergo additional testing, specifically magnetic resonance imaging (MRI) of the abdomen.
While the MRI did indeed reveal a treatable infection that explained Lindsey’s continuing symptoms, it also revealed something much more alarming and unexpected.
Lindsey had a two-inch-long tumor on her pancreas.
Transferred to Mass General
Dr. Masiakos immediately called Lindsey’s parents to break the news that he had discovered a mass on their daughter’s pancreas.
“[He] called us on the phone and asked if we were alone, and he shared with us that Lindsey had a tumor on her pancreas,” says Emily. “He said that we’re going to take it one step at a time. We would first give Lindsey some time to recover from her appendectomy and then, when she was ready, she would be transferred downtown to Massachusetts General Hospital.”
Dr. Masiakos’ decision to transfer Lindsey to Mass General ensured that he would remain an active member of her surgical care team, while also positioning her as a patient in an institution that is home to one of the top-volume programs for general pancreatic care.

While Lindsey recovered from her first surgery, Dr. Masiakos consulted with Motaz Qadan, MD, PhD, a pancreatic surgeon at Mass General, who reviewed the MRI imaging and confirmed that her tumor was a non-cancerous (benign) distal pancreatic tumor located at the tail end of her pancreas.
Both Dr. Masiakos and Dr. Qadan agreed that pancreatic surgery would need to wait until she had adequately recovered from her infection, as the excessive inflammation could comprise the pancreatectomy.
“We had to balance allowing Lindsey enough time to recover from an inflammatory process that could cause complications in a pancreatic operation and not waiting too long to address the tumor that could be growing,” says Dr. Masiakos.
As summer turned to fall, Mark and Emily grew anxious to confirm the next steps in their daughter’s care. Dr. Masiakos assured them that the delay in proceeding with pancreas surgery was in pursuit of the best possible outcomes for Lindsey, and immediately connected them with Dr. Qadan to provide answers to their questions about the surgery itself.
“Dr. Qadan called me that very same day,” Emily says. “And the first thing he said to me on the phone was, ‘I’m really sorry that you have to go through this.’ And immediately I felt like this is a compassionate man who is going to take care of our daughter.”
After discussing as a team, Dr. Masiakos, Dr. Qadan, and her parents agreed that Lindsey’s surgery should take place that fall at a time that would ensure minimal interference with her school.
High-volume Expertise, Combined Care
Mass General is home to the fastest-growing robotic surgery program in New England, and the surgical team decided that Lindsey’s condition would be best treated robotically. Their decision to use the robot to remove the tumor on Lindsey’s pancreas was two-fold.
“I knew that I wanted to do [her surgery] minimally invasively so that she could recover much faster and return to her normal activities more quickly,” says Dr. Qadan. “And then in doing this robotically, our goal was also to preserve the blood vessels that go to the spleen and, in doing so, preserve her spleen.”
Pancreatectomies often involve removing the spleen, leaving patients at increased risk of infection. However, because of the size of her mass and its position on her pancreas, Lindsey was able to undergo a spleen-sparing pancreatectomy — a surgical approach regularly performed by the highly specialized team at Mass General.
Both the pediatric and pancreatic surgical teams were in the operating room together for Lindsey’s surgery, allowing for expertise on both sides to collaborate under one roof. Dr. Masiakos marked out the spots for where the robotic instruments would enter Lindsey’s abdomen — through her belly button to ensure the least possible scarring. With the robot, Dr. Qadan precisely and expertly peeled the tumor off her pancreas without disrupting the spleen.
“We were actually able to extract the tumor straight from Lindsey’s belly button, which meant very minimal scarring,” says Dr. Qadan. “We then closed her up and went to tell her parents the good news — we’d gotten out all of her tumor without needing to remove her spleen.”
Back at School Four Days After Surgery
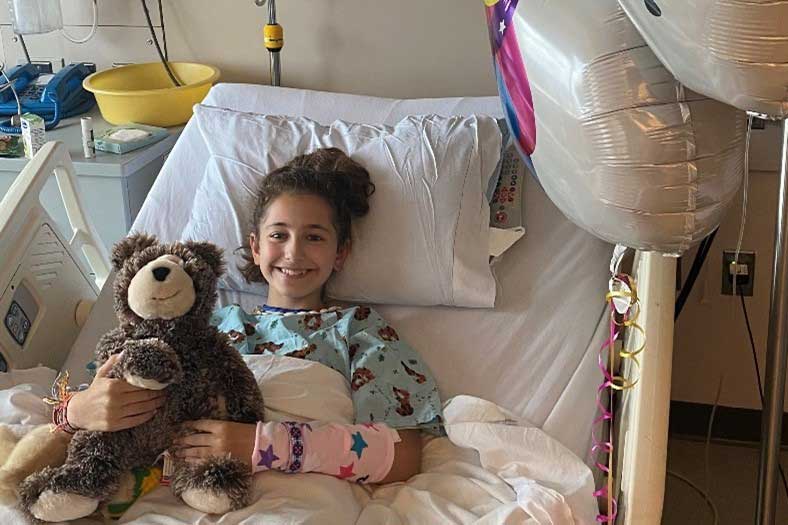 As is typical for pancreatectomies, Lindsey remained at Mass General to recover after her surgery. However, much to the surprise of her parents, she was discharged a short four days later without any sign of pain, enabling her to return to school less than a week after surgery.
As is typical for pancreatectomies, Lindsey remained at Mass General to recover after her surgery. However, much to the surprise of her parents, she was discharged a short four days later without any sign of pain, enabling her to return to school less than a week after surgery.
Using the robot to perform the surgery, Dr. Masiakos asserts, was absolutely the right choice for Lindsey’s condition. “If I had to do it again, I would do it the very same way,” he says.
Today, almost two years later, Lindsey is enjoying an active, normal life for a 13-year-old. She has since returned to her favorite summer pastime of sleepaway camp and her family’s shared hobbies of playing board games and baking desserts.
“It’s just tremendous how well the different subspecialties [at Mass General] work together as a true team,” says Emily. “As a parent, all you want to do is protect your child, and they took care of our daughter in ways that we couldn’t. And it felt like they did it like she was their own child. That’s all we could ever ask for, and we’re so grateful.”
-
![]()
- Director, Pediatric Trauma Services
- Co-Director, MGH Center for Gun Violence Prevention
- NWH Chief of Pediatric Surgery
-
![]()
- Surgeon-in-Chief, Mass General Brigham Cancer Institute
- Gapontsev Family Endowed Chair in Surgical Oncology
Type
Centers and Departments
Topics
High-volume often means better outcomes
Our high-volume practice and highly specialized team help us attain excellent results when treating common and complex conditions of the pancreas.
Surgical Outcomes for Pancreatic Conditions
Mass General provides its outcomes and performance data for surgical treatment of pancreatic conditions including cancer and necrotizing pancreatitis.
Exceptional Pediatric Care
A new model for children's health care: learn more about Mass General Brigham for Children.
Robotic Surgery
Mass General is home to the fastest growing robotic surgery program in New England and is a minimally invasive treatment option for many conditions.
Appointments and Referrals
Request an appointment or second opinion, refer a patient, find a doctor or view test results with MGfC's secure online services.



