Patient StoryDec | 7 | 2020
Michael’s Story: Duodenal Atresia
 At Briana Fiorante’s 24-week ultrasound, doctors at Holy Family Hospital in Methuen, Massachusetts, found signs of duodenal atresia, commonly known as a “double bubble,” a condition in which the duodenum, part of the small intestine that connects to the stomach, has a blockage that prevents food and fluids from passing through the body. Briana and her husband, Joe, were immediately referred to the Mass General for Children (MGfC) Fetal Care Program and the Mass General Maternal Fetal Medicine Program, and Briana’s care was transferred to William Barth, MD, vice chair of Obstetrics at MGH.
At Briana Fiorante’s 24-week ultrasound, doctors at Holy Family Hospital in Methuen, Massachusetts, found signs of duodenal atresia, commonly known as a “double bubble,” a condition in which the duodenum, part of the small intestine that connects to the stomach, has a blockage that prevents food and fluids from passing through the body. Briana and her husband, Joe, were immediately referred to the Mass General for Children (MGfC) Fetal Care Program and the Mass General Maternal Fetal Medicine Program, and Briana’s care was transferred to William Barth, MD, vice chair of Obstetrics at MGH.
“It happened quickly,” says Briana. “Other factors could be involved in the condition, so we had appointments every two weeks. We had fetal echocardiograms and a trisomy test, but thankfully, everything came back fine.
Karen Parson, RN, nurse coordinator for the MGfC Fetal Care Program, became Briana’s guide and helped the family understand and manage their prenatal diagnosis. The Fetal Care Program’s nurse coordinators help families navigate the health care system and ensure they have the information and resources they need. Additional fetal care team members include pediatric cardiology and surgery physicians.
“Karen stuck out to me right away,” says Briana. “At some point, things can fall through the cracks. From the beginning, she was phenomenal and knew what we needed. Parsons scheduled the Fiorante’s many appointments all in one day, minimizing their long trips to Boston. They consulted with Cassandra Kelleher, MD, surgical director of the Fetal Care program, to discuss how their newborn son, who would be named Michael, would be treated after birth.
“We wanted answers right away, but Dr. Kelleher and Karen had a plan. Everything was almost instant. We got results before leaving the exam room. It was comforting,” says Briana.
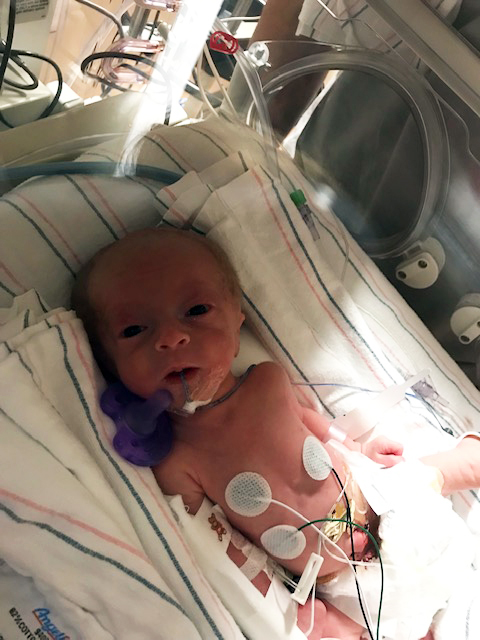
Michael was born via vaginal delivery on April 27, 2018, after Briana went into unplanned, preterm labor at 32 weeks gestation. Pediatricians were present at his delivery and he was transported to the Neonatal Intensive Care Unit (NICU) soon after delivery. After delivery, Briana’s placenta did not deliver spontaneously, a condition known as retained placenta. Andrea Edlow, MD, MSc., a maternal-fetal medicine specialist, worked with obstetrics anesthesia and nursing staff to successfully remove the placenta without the need for additional procedures. Briana met Michael in the NICU the following day.
The newborn weighed only 3 pounds and was placed in an incubator to regulate his temperature and treat jaundice, a yellowing of the skin. He quickly began to gain weight during his four week stay in the NICU and at discharge, tipped the scale at 4.6lbs.
Since there are no treatments for duodenal atresia prior to birth, newborns — such as Michael – typically undergo surgery within 1 – 3 days after birth to repair the connection between the stomach and intestines. Though he was not able take a bottle before the surgery was performed, Michael received all necessary calories and nutrients through an IV. Though some babies continue to experience a slow progression of food through their intestine after surgery and require additional medicine to assist in digestion, Michael learned to eat all his food by mouth and did not need additional assistance.
Michael, now 2 ½ year old, is thriving. He loves trucks, tractors and animals. There have been no complications from the surgery to repair his duodenal atresia, though the Newborn Developmental Follow-Up Clinic will follow Michael’s case for any potential duodenal atresia complications.
“No parent wants to see their child sick,” says Briana. “but if it had to happen, MGfC is where I’d want to be treated. We didn’t have a choice, but we had a good experience. We are forever MGfC patients.”
Related Centers/Departments
Type
Centers and Departments
Topics
Exceptional Pediatric Care
A new model for children's health care: learn more about Mass General Brigham for Children.

