Understanding Child Stroke
Explore This Condition
Kinds of Strokes
Not all strokes are the same! Blood flow to the brain can be compromised in different ways that give rise to the type of stroke.
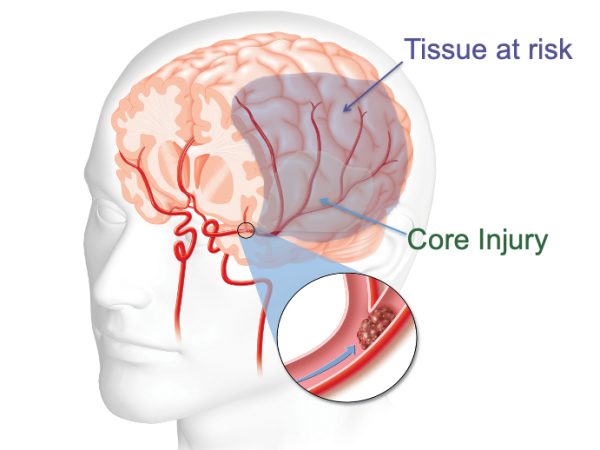
Ischemic Strokes occur when a blood vessel that supplies or drains the brain is narrowed or blocked, slowing down the blood supply to that part of the brain that depends on them. Loss of blood flow is called ischemia.
Most commonly it is caused by clots (thrombi) or fat plaques (atherosclerotic plaques) affecting an artery. These can originate at the site of the blockage – thrombotic – or can occur when a clot or other debris travel from somewhere else (the heart, a neck vessel) and lodges in a smaller artery interrupting the blood supply (embolism or thromboembolism). Another mechanism of ischemic stroke occurring in people affected by previously narrowed cerebral vessels (moyamoya or other vasculopathies) are low blood pressure states (i.e. dehydration, anesthesia) or vasoconstriction/squeezing of those affected vessels during exposure to certain medications.
Common causes leading to arterial ischemic stroke in the young include cerebral artery dissection, heart conditions such as congenital heart disease and patent foramen ovale (PFO), the reversible cerebral vasoconstriction syndromes, infections like HIV and TB, genetic conditions, drug abuse, blood disorders, and cancers.
Blood flow can also slow down or stop if the vein draining that part of the brain is blocked by clotting (venous thrombosis). This is called venous ischemia and tends to be less severe if the build-up pressure in the system does cause rupture and bleeding.
Hemorrhagic Strokes occur when a blood vessel in your brain leaks or ruptures inside the brain. Bleeding in the brain causes pressure to the nerve cells and comprises their survival. The bleeding can originate from arteries or veins inside or around the brain. Common causes include the rupture of brain aneurysms, subarachnoid hemorrhage, arterial malformations, blood disorders, the reversible cerebral vasoconstriction syndromes, cerebral venous sinus thrombosis and drug abuse.
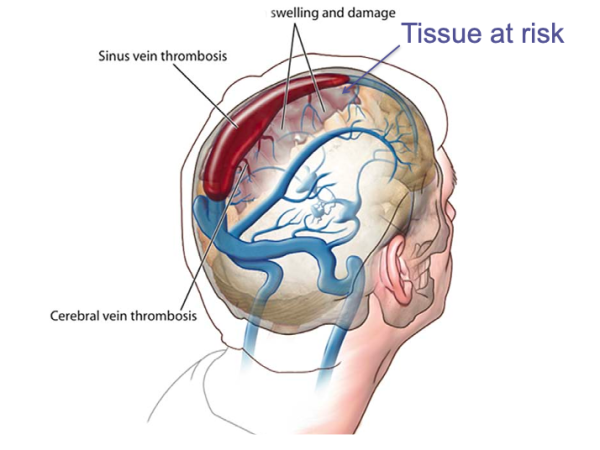
Cerebral Venous Sinus Thrombosis (CVST) occurs when blood flow slows down or is blocked by a blood clot (called a venous thrombosis) in the vein that drains the brain. Lack of blood flow in this region is called venous ischemia and tends to be less severe if the build-up in pressure from the blockage does not cause rupture or bleeding. It is possible for the pressure to become too high, causing damage to the vessel and forming a hemorrhage.
Periventricular Venous Infarct (PVI) can happen when there is a blockage of the blood flow that does not affect the outer part of the brain (cortex) and only sustains injury to the inner most area.
Transient ischemic attack (TIA) resembles a stroke, producing similar symptoms, but usually lasts only a few minutes and causes no permanent damage. It occurs due to the temporary blockage of an artery to the brain by a thrombus, that spontaneously passes once again, restoring blood flow to the brain.
What is Unique about Stroke in Children and Newborns?
Pediatric stroke is NOT the same as adult stroke. As a child grows, the brain develops at a remarkable rate—especially during infancy! During this time, neurons are creating, destroying, strengthening, and weakening connections amongst themselves. These connections, or synapses, create work to allow humans to do all that we do. The type of synapses and the ways they are formed are influenced by infants’ experience and biology. The brain’s ability to change in response to different environmental factors is called plasticity. Plasticity is particularly important when thinking about pediatric stroke. The brain’s more generous plasticity during childhood allows it to respond quickly to the consequences of stroke—thereby ensuring that brain development and functions continue normally. While adult brains are capable of plasticity as well, it is often more difficult for the brain to respond as effectively to such injuries.
Newborns and Infants
If your newborn has been diagnosed with a stroke, close monitoring, control of seizures and evaluations are necessary to prevent further injury to the brain and optimize the changes of his/her neurological development and recovery. It is very important that your baby is evaluated by a Pediatric/Perinatal Stroke Team as soon as possible. You can request to speak with the specialist in the hospital you are at or request a transfer to a hospital with pediatric stroke services.
What can cause stroke in infants and children?
While stroke in infants and children is rare, it may not be as rare as you suspect. Stroke in these populations are more common than brain tumors, and by some estimates, as frequent as strokes in the elderly. The most common type of stroke in infants is called an arterial ischemic stroke (AIS). This happens when a clot blocks blood flow to major brain arteries. These clots can form at the location of blockage or in another place, such as the placenta or heart, and travel to the child’s brain. Other, less common, types of stroke in children include cerebral sinus venous thrombosis (CVST), where there is blockage of blood flow in brain veins, and periventricular venous infarction (PVI), which does not affect the cortex and only affects the inner most part of the brain. There are certain risk factors such as cardiac abnormalities, infections, complicated delivery or a genetic mutation that can contribute to stroke in infants; however, a clear explanation has yet to be determined as each case is unique.
Stroke and Child Brain Development
One of the most important ways that child stroke is different from adult stroke is that a child's brain is still developing rapidly, especially during infancy. During this time, neurons are creating, destroying, strengthening, and weakening connections amongst themselves. These connections, or synapses, create functional units that allow humans to do all that we do. The types and ways in which synapses form are influenced by infants’ experience and biology. The brain’s ability to actively change in response to different environmental factors is called plasticity. Plasticity is particularly important when thinking about pediatric stroke. The brain’s more generous plasticity during childhood allows it to respond quickly and effectively to the consequences of stroke—thereby ensuring that brain development and functions continue normally. While adult brains are capable of plasticity as well, it is often more difficult for the brain to respond as effectively to such traumas.
Despite the greater plasticity of the young brain, at least 50% of perinatal stroke survivors experience long term neurological impairment such as hemiplegia (paralysis on one side of the body), hemiparesis (impaired movement on one side of the body) and language and learning difficulties. Other common effects include epilepsy, emotional and behavioral challenges, visual or sensory impairments and balance problems. In some cases, feeding issues, constipation, hearing problems, slow growth, hydrocephalus and scoliosis have been reported.
Stroke in Young Adults
What is Unique about Stroke in the Young?
While stroke is one of the most common diseases, suffering a stroke under the age of 60 may suggest evidence for a hereditary cerebrovascular disorder. Compared to its effect on older people, stroke causes a disproportionally higher impact on the life expectancy and quality of life in young people. The longer length of disability, loss of independence and handicap during these productive years, together with the risk for disease progression and new strokes, make these patient populations extremely burdened and vulnerable.
This is why it is so important to manage a stroke during young adulthood with specialists including medical and therapy providers. Due to the possibility of other conditions underlying the cause of stroke it is important for individuals to seek stroke specialists who may be able to provide future monitoring.
What can cause Stroke in Young People?
Unlike stroke in the elderly, heart disease, hypertension or diabetes are not usually the culprit with lipid, blood and vessel disorders contributing to a majority of cases of stroke in young people. Underlying each of these contributing factors is a possibility of a genetic mutation or disorder. If you know a genetic mutation in your family that can cause any of these it is important to consult a stroke team to better understand the ways you can prevent stroke. Similarly, if, after a stroke, you are found to suffer any genetic condition that had put you at a predisposition, it is important to consult these specialists to manage further stroke prevention.
The most common type of stroke young people is called an arterial ischemic stroke (AIS). This happens when there is a clot or critical narrowing of vessels that blocks blood flow to major brain arteries. Clots can form at the location of blockage or in another place, such as the heart, and travel to your brain. This interruption of blood flow can cause you to have blurred vision, slurred speech, and numbness, tingling or weakness in your face, arms, and legs (as listed below). Other types of injuries include cerebral sinus venous thrombosis (CVST), where there is blockage of blood flow in brain veins, and periventricular venous infarction (PVI), which does not affect the cortex and only affects the inner most part of the brain. Understanding the type of stroke you had is important for your future care and injury prevention.
Can Genes Cause Stroke?
Stroke is one of the leading causes of death in people over 55 with many cases of stroke due to the effects of aging; however, young people do not normally possess risk factors such as atherosclerosis (vessel plaque build-up) or high blood pressure putting this population at a lower risk. Incidence of stroke in children and young adults raises the question of what other factors, such as genetics, may be contributing to young strokes. The clearest evidence that genetic factors may be involved in the pathophysiology of stroke in these young people arises from monogenic forms of the disease, where a single gene leads to dysfunction, increasing the risk and recurrence of ischemic or hemorrhagic strokes. These single-gene disorders lead to problems including but not limited to lipid, blood clotting, or vessel dysfunction. It is also possible that a stroke can be caused by the interaction between multiple genes, this is called a polygenic cause. Often, individuals do not find out they have a genetic disease until after an event such as a stroke. Learning about one’s disease state is critical for proper health management and minimizing the risk of future events.
Seeking a Genetic Diagnosis with Genetic Counseling
Genetic counseling is a process to evaluate and understand a family’s risk for an inherited medical condition and provides information and support to people who have, or may be at risk for, genetic disorders. A genetic counselor is a healthcare professional with specialized training in medical genetics and counseling.
There are many reasons that people go for genetic counseling, such as:
- If there is a family history of a genetic condition;
- To learn about genetic screening for diseases that are more common in certain ethnic groups (e.g., sickle cell disease in African Americans)
- To discuss abnormal results from tests during pregnancy
- If a woman has had several miscarriages or infant deaths
- If a genetic condition or birth defect occurred in a previous pregnancy
- If a child has birth defects, disabilities, or conditions found by newborn screening
- To find out if there is a genetic cause for developmental delays or health problems.
Healthcare providers can help their patients find a genetic counselor or clinical geneticist in their area. The nearest medical school or university medical center will usually have information about finding a genetic professional.
These websites may help you locate a board-certified genetic specialist nearby:
Exome Sequencing
Exome sequencing can be helpful for people who do not have a diagnosis. The “exome” is the component of the genome that codes for the protein. The exome comprises about 1% of the genome and is, so far, the component most likely to include the mutations that result in clinical phenotypes (signs of the disease expressed in people). Whole exome sequencing involves determining the DNA sequence of most of these protein-encoding exons. The goal of this approach is to identify genetic variants that change protein sequences. It is possible that some clinically significant mutations may be missed as the technology is changing, but this is the best way to identify known-mutation causing diseases at this time.
Genetic Conditions That May Cause Child Stroke
Child stroke may be caused by a wide range of factors but there are some genetic conditions that make it more likely, including some genetic conditions. The Young Genetic Stroke Alliance provides detailed information and extensive resources to families with genetic stroke disorders.
Conditions that make pediatric stroke more likely include:
- Genetic Thrombophilias: genetic mutations that cause blood to clot abnormally.
- Sickle-cell anaemia: a disease in which the body’s hemoglobin has an irregular shape, which can cause blood clotting and blocked vessels.
- MoyaMoya: a rare, progressive disease in which arteries are blocked in a region of the brain called the basal ganglia.
- Vascular Malformations: an abnormal connection between the arteries and veins in the brain that usually forms before birth.
- Fabry disease: a genetic disease that causes an excess of fat buildup in the body’s cells. Complications can lead to stroke.
- Homocystinuria: a genetic disease in which the body is unable to process certain proteins, and so increases the risk of blood clotting.
- Marfan syndrome: a genetic disorder in which the proteins of connective tissue are mutated. This can cause a variety of symptoms depending on affected tissues, including stroke.
- Ehlers-Danlos syndrome: a genetic disorder that encompasses a group of connective tissue disorders, primarily focused on mutations in collagen and its associated proteins. This disease can lead to a variety of symptoms, including stroke.
- CADASIL/CARASIL (Cerebral Autosomal Dominant Arteriopathy with Sub-cortical Infarcts and Leukoencephalopathy): a genetic disease that causes the walls of blood vessels to thicken, and so prevent blood flow.
- Mitochondrial Encephalomyopathy, lactic acidosis, and stroke-like episodes (MELAS): a disease caused by mutant mitochondria that affects both the nervous system and muscles. It is often characterized by a buildup of lactic acid, and often causes stroke.
- Loeys-Dietz Syndrome: a genetic disorder that affects the connective tissue in many parts of the body. Connective tissue provides strength and flexibility to structures such as bones, ligaments, muscles, and blood vessels (http://ghr.nlm.nih.gov/condition/loeys-dietz-syndrome).
- ACTA2: a genetic disorder that causes multisystemic smooth muscle dysfunction. This disorder impairs the activity of smooth muscles throughout the body and leads to widespread problems including blood vessel abnormalities (most commonly involving the aorta), decreased response of the pupils to light, a weak (hypotonic) bladder, and impairment of the muscle contractions that move food through the digestive tract (hypoperistalsis).
- Atrial Fibrillation: An irregular heartbeat, which can lead to blood clotting and blocked vessels.
Strokes Can Happen at Any Age
Pediatric stroke can happen in infants, children and even before birth. Learn more from the American Stroke Association.
Los Ataques Cerebrales Pueden Ocurrir a Cualquier Edad
Pueden sucederle a bebés, niños e incluso a neonatos. Aprende más con este folleto del American Stroke Association.
Support Our Work
Your gift will support comprehensive, compassionate clinical care and innovative research to help for children recovering from stroke.




