Young Adult With Congenital Heart Disease Has Completed Three Marathons…and Counting
Alexa, born with tetralogy of Fallot, thrives today as a nurse and marathon runner thanks to adult congenital heart disease care at Mass General Brigham.
Corrigan Minehan Heart Center
Contact Information
Corrigan Minehan Heart Center
55 Fruit Street
Boston,
MA
02114
Phone: 866-644-8910
Specialists in the Heart Valve Program at the Massachusetts General Hospital Corrigan Minehan Heart Center work closely with patients and referring physicians to determine the treatment plan that is best for each patient. Not all patients with mitral valve regurgitation are candidates for the minimally invasive mitral valve repair (see below for eligibility).
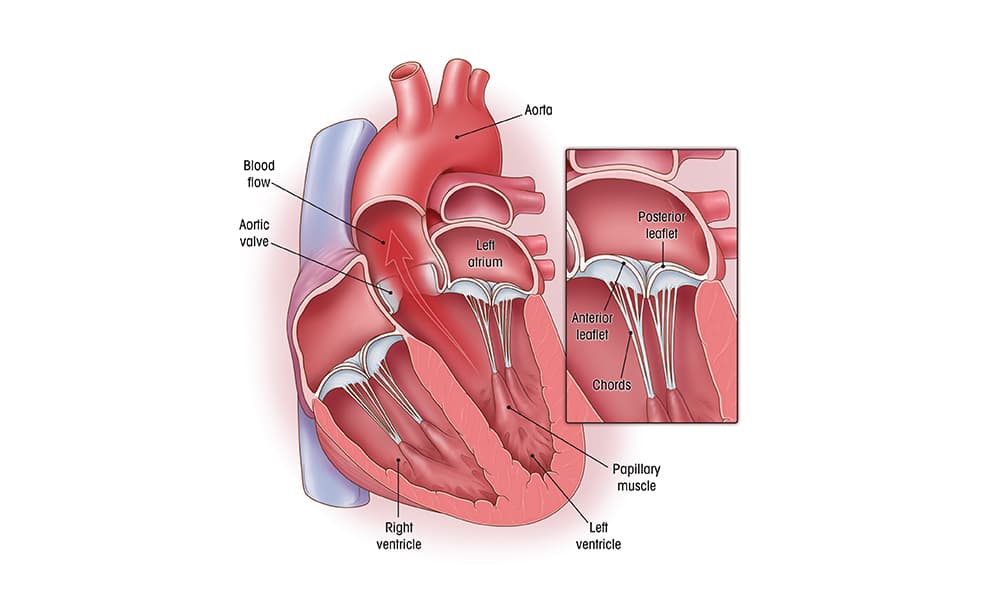
The heart has four valves: mitral valve, aortic valve, tricuspid valve and pulmonary valve. The valves ensure that blood flows in one direction through each of the heart's four chambers, and then out of the heart and into the body.

View of a normal mitral valve.
The mitral valve has two leaflets (anterior leaflet and posterior leaflet) that open and close to let blood pass from the left atrium (upper chamber) to the left ventricle (lower chamber).
When the mitral valve fails to close and seal completely (mitral valve prolapse being the most common), blood flows backwards into the upper chamber. This condition, known as mitral valve regurgitation (or mitral insufficiency), is one of the most common forms of heart valve disease.

Image of mitral valve prolapse.
Severe mitral valve regurgitation can cause the heart to enlarge over time and pump blood less effectively. As a result, patients may develop heart failure and experience symptoms such as:

Image of a broken mitral valve from the left atrium.
In some cases, a patient may need to undergo valve replacement surgery. Other times, the mitral valve can be repaired in a couple of different ways:
In either approach, the mitral valve is analyzed and repaired in a step-wise manner. Various techniques are available to the surgeon in order to make the valve competent again.
Patients with severe mitral regurgitation where mitral surgery is not recommended (for example, patients with very high surgical risk) may be candidates the MitraClip system. This procedure uses a small clip to repair the heart's mitral valve to treat mitral regurgitation. The clip is inserted through the venous system without any chest incisions.
Mitral valve repair involves reconstructing the mitral valve leaflets so that the leaflet edges meet and properly seal again. This usually entails either a removal of the flail portion of the leaflet (the portion not supported by the ruptured/broken chords) or placement of new chords—or both in some complex cases.
Repairing the mitral valve rather than replacing it with an artificial valve may prevent the need for lifelong use of blood-thinning medications. It also preserves the internal structure of the heart, which may keep patients healthier in the long run.
Two different mitral valve repair techniques may be used. In both techniques, small incisions are made in usually the right chest wall so that the surgeon can insert small instruments to repair the valve.
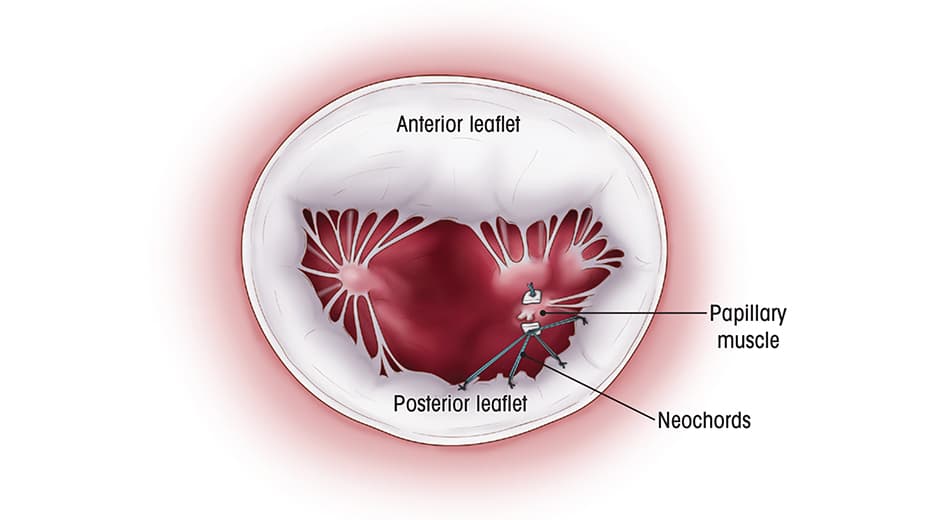
View of repaired mitral valve using the neochordal technique from the left atrium.
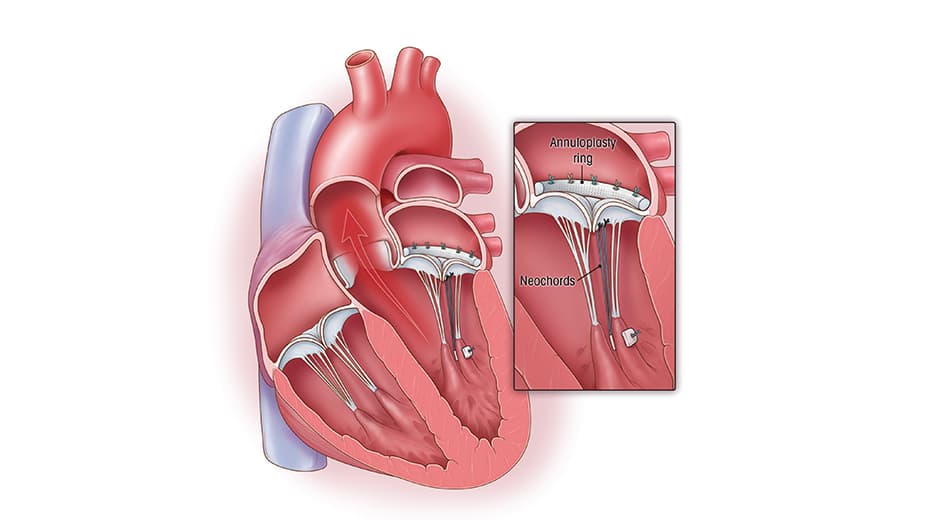
Repaired mitral valve using the neochordal technique
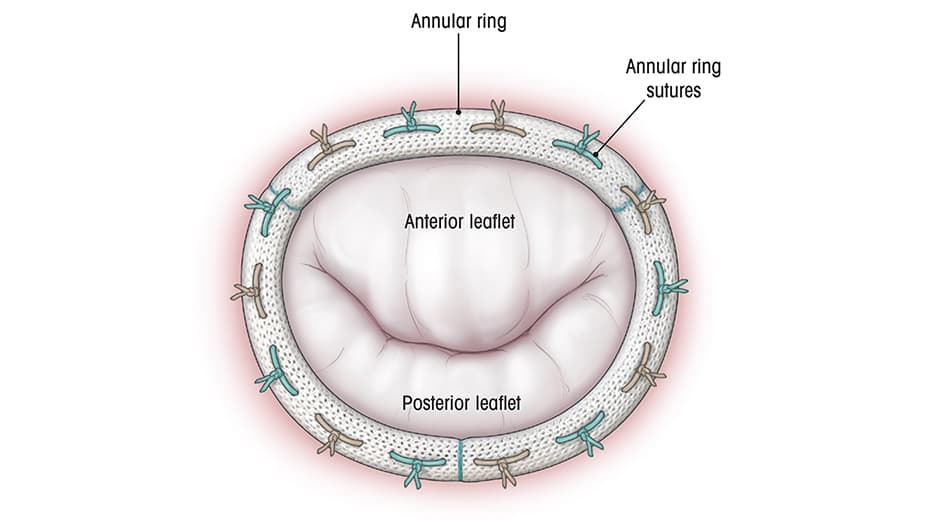
Final result of the repaired mitral valve using the neochordal technique.
Compared with traditional open surgery (sternotomy), minimally invasive procedures tend to result in:
Not all patients are candidates for the minimally invasive mitral valve repair approach. Some might require another procedure on their heart, such as a coronary artery bypass grafting procedure, and therefore would need to undergo their surgery through a traditional sternotomy approach.
Some patients may not be candidates for the minimally invasive approach due to other conditions that may be present, such as:
Eligibility is discussed in detail during the preoperative clinic visit.
The surgery itself is safe and carries a low complication rate. The success rate is similar to conventional mitral valve repair. More than 95% patients who underwent minimally invasive mitral valve surgery at Mass General had a successful mitral valve repair.
Patients meet with members of the Heart Valve Program care team to discuss the best treatment approach.
Prior to the minimally invasive mitral valve repair surgery, the patient will be asked to undergo a test to better assess the coronary arteries of the heart. This can be done either by coronary catheterization (a minimally invasive procedure used to access the coronary circulation of the heart using a catheter) or by a special computed tomography (CT) scan and will be further discussed during the preoperative discussion with the care team.
After the surgery, the patient generally stays one to two days in the intensive care unit and two to four days on the regular postoperative floor. Patients are given clear instructions prior to the discharge home or to rehabilitation as well as a follow-up appointment with the surgeon and their cardiologist.
Depending on the approach and patient’s overall health, recovery after the surgery can be as short as four to six weeks or can require up to three months.
Dolly's Story: Getting Back on Her Feet
When mitral valve disease started to affect the quality of Dolly Lakkis' life, she turned to a team of Mass General specialists. Dolly’s doctors repaired her damaged heart valve with minimally invasive surgery, that got her back on her feet—and back on the dance floor—as quickly as possible.
With Mass General Brigham, patients gain access to a world-class system of specialized heart and vascular experts.
Virtual visits allow you to conveniently meet with your provider from home—either online (over your computer or device) or by phone.
Our physicians welcome second opinion appointments to review cases and proposed lines of treatment.
Alexa, born with tetralogy of Fallot, thrives today as a nurse and marathon runner thanks to adult congenital heart disease care at Mass General Brigham.
Did you know that your mental well-being affects more than just your mood? New research shows that living with depression or anxiety may put your heart at risk, too.
J. Sawalla Guseh, MD, a Mass General Brigham sports cardiologist and director of the Cardiovascular Performance Program at Massachusetts General Hospital, explains that your heart rate is a key metric for improving your fitness.
Researchers from Mass General Brigham will present discoveries and outcomes from clinical trials and research studies for cardiovascular conditions, including heart disease and heart failure, at the European Society of Cardiology (ESC) Congress, being held in Madrid, Spain, from Aug. 29–Sept. 1.
Uncontrolled blood pressure puts people at increased risk of developing heart disease, brain disease, and kidney disease, yet only one in four people have their blood pressure under good control.
New study shows that being sedentary increases the risk of the most common types of heart disease, even among those who get enough exercise
Call us to learn more, or request an appointment online.