Center for the Neuroscience of Psychedelics

Contact Information
Center for the Neuroscience of Psychedelics
Learn More About This Center
Overview
Mental illness is the leading cause of disability in developed countries. Fifty percent of Americans experience mental illness in their lifetime and $350 billion is spent annually on treating depression in the U.S. and Europe alone.
Nearly half of that total represents the cost of treatment-resistant patients: those who do not improve despite multiple treatments.
One of the biggest clinical challenges in mental health is treatment resistant patients: those who seek help, but do not improve despite multiple medication and treatment intervention trials.
Treatment resistance reflects both the limitations of our currently available treatments, as well as the likelihood that these patients’ brains are less capable of change in ways that improve mental health.
Please note that psychedelics and psychedelic-assisted therapy, at present, are not FDA-approved treatments and are not available for clinical use (except for ketamine). Our Center, which conducts scientific research, is only able to provide psychedelic assisted psychotherapy in the context of a research study.
If you are interested in ketamine treatment at MGH please check out the website for the Mass General Ketamine Clinic. Please note that at this time they do not offer ketamine-assisted psychotherapy.
Neuroplasticity and Healing
Our treatments work by bringing about changes in the brain—it is the brain’s neuroplasticity, or capacity for change, that makes healing possible.
Read more
Neuroplasticity is seen at the cellular level, at the level of neurons, all the way up to changes in networks of brain regions underlying behavior.
Some of the factors that help make the brain more receptive to change are in lesser supply in patients suffering from depression and suicidal ideation. This reduces their brain’s capacity to change and adapt to the environment. For our patients with treatment resistance, this problem is magnified.
The key to solving the biggest challenge in mental healthcare is to increase the brain’s capacity for change, to promote healing and eventually wellness.
The Promise of Psychedelic Medicines
Psychedelic compounds—in particular psilocybin, 3,4-methylenedioxymethamphetamine (MDMA) and N,N-Dimethyltryptamine (DMT)—have emerged as promising treatments that may increase the brain’s capacity for change.
Studies suggest that psychedelics may facilitate neuroplasticity at the cellular and network levels allowing the brain to form and reorganize connection.
This creates a unique opportunity to change patterns in brain activity, and in turn, improve symptoms, behavior and functioning, to ultimately eliminate suffering.
There is much to learn about how these psychedelic compounds work in the brain to promote neural plasticity. Initial clinical studies suggest immediate, sustained relief of symptoms after a single administration of a psychedelic compound in a therapeutic setting.
Our Research
Remarkable advances in brain imaging—many pioneered and developed at Mass General—allow scientists the unique opportunity to leverage the world’s most advanced neuroimaging tools and methods to see the neuroplastic effects of psychedelic drugs from neurons to networks.
Seeing and understanding these changes in the brain offers an unprecedented possibility to rapidly transform mental health research and treatment.
The knowledge of how psychedelics promote this sort of change, or neuroplasticity, can be harnessed to complement and even enhance current treatments and alleviate the suffering of those patients in the greatest need of help—and hope.
Comprehensive Interdisciplinary Approach
The Center brings together leaders in psychiatry, chemical neurobiology, and neuroimaging.
Our team of clinicians, clinician scientists, neuroscientists and medical physicists collaborate to investigate the effects of psychedelics at the molecular, cellular and systems levels across different patient populations. Our ultimate goal is to promote healing and alleviate patient suffering.
The Center will leverage Mass General's tradition of excellence, which attracts a global array of stakeholders from academia, industry, and the non-profit world to promote and accelerate collaboration and increase the impact of psychedelic research. The center operates in an extraordinary biomedical and biotech ecosystem that includes Mass General, Harvard Medical School, Harvard University and the Broad Institute along with dozens of biotechnology and biopharmaceutical companies.
- Department of Psychiatry
- Mass General's Department of Psychiatry is ranked #1 in the United States per U.S. News and World Report.
- It is home to more than 60 specialty clinics and research programs and has the largest clinical research program at Mass General, with studies at the forefront of neuroscience, molecular biology, and genetics.
- Chemical Neurobiology Laboratory
- At the cellular and molecular level, Stephen J. Haggarty, PhD, leads efforts in the chemical neurobiology laboratory.
- Dr. Haggarty’s group applies precision medicine approaches to understand the molecular and cellular mechanisms of brain plasticity that underlie the beneficial effects of therapeutic psychedelics.
Read more about the Chemical Neurobiology Lab
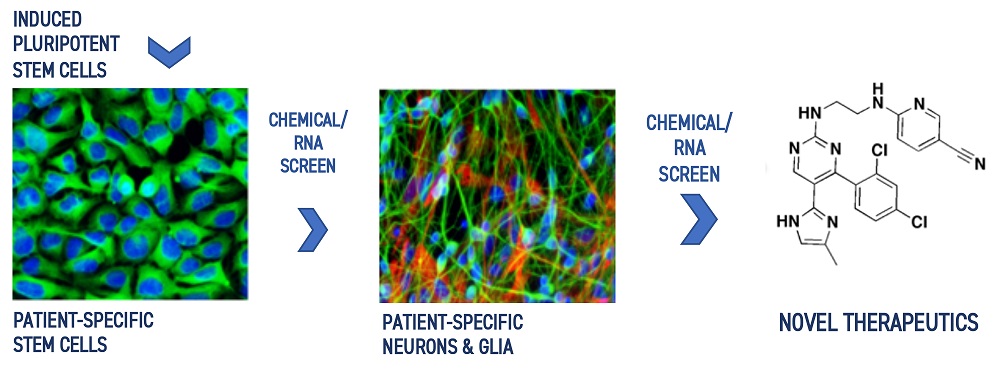
Using patient-specific stem cell-derived organoids, his group explores the effects of psychedelic compounds to help identify cellular and molecular markers of treatment response to advance the discovery of next generation therapeutics targeting brain plasticity and health.
- Athinoula A. Martinos Center for Biomedical Imaging
- The Athinoula A. Martinos Center for Biomedical Imaging at Mass General, led by Bruce Rosen, MD, PhD, is one of the world’s premier research centers devoted to the development and application of advanced biomedical imaging technologies.
Read more about the Martinos Center
Led by Bruce Rosen, MD, PhD, a pioneer in the development and application of functional MRI techniques, the imaging capabilities and scientific team at the Martinos Center is unmatched anywhere else in the world.
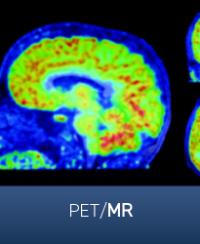
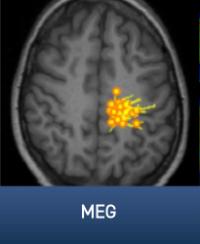
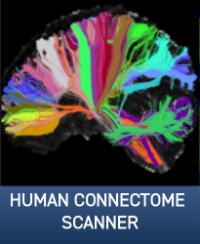
At the level of brain regions, circuitry and networks, Drs. Ghaznavi and Rosen will work in close concert to bring together the latest in cognitive neuroscience and neuroimaging to study how changes in the brain brought about by psychedelics relate to changes in the way people think, feel and function.
Current Research
Our foundational research studies aim to understand how psychedelics facilitate changes in brain structure and function, with an initial focus on psilocybin for patients with treatment-resistant depression.
For all studies, we will collect a wide array of neuroimaging data to fully understand the neural correlates of change with psilocybin.
- The Center's first study, led by Dr. Sharmin Ghaznavi, will explore psilocybin's effect on rumination, a process which contributes to depression, anxiety, and other mental illnesses. Please refer to our listing on ClinicalTrials.gov.
If you are interested in participating in this research study, please contact cnpcogneuro@mgh.harvard.edu. - In conjunction with the MGH Division of Gastroenterology’s Center for Neurointestinal Health, the CNP is exploring psilocybin-assisted therapy as a treatment for irritable bowel syndrome (IBS.) IBS is a pain disorder characterized by disordered gut-brain communication. This study is led by Erin Mauney, MD, Franklin King, MD, and Brad Kuo, MD. Please refer to our listing on ClinicalTrials.gov.
If you are interested in participating in this research study, please contact GIMotilityResearch@mgh.harvard.edu.
Schultes Legacy Project
Toward Next-Generation Neurotherapeutics Targeting Neuroplasticity
While psychedelics have been used by humans for millennia, the field of modern therapeutic psychedelics has its origins due to the pioneering work of ethnobotanists and natural product chemists. Central among these early investigators is the late Harvard Professor Richard Evans Schultes, PhD. Widely considered the founding father of the field of ethnobotany, Schultes was director of the Harvard University Herbaria & Botanical Museum. The Center will investigate the therapeutic potential of the hundreds of plants that hold promise for a wide range of range of indications.
Watch the webinar
Read more
As a professor of botany at Harvard, he inspired and trained a generation of scientists to document and protect indigenous cultures, as well as champion the preservation of environmentally sensitive places like the Amazon Rainforest where much of his fieldwork was completed. Schultes’s innumerable ethnobotanical discoveries, starting in the late 1930s and throughout his career, helped lay the foundation for the field of psychedelic research. He curated observations of the human uses and properties of approximately 100 psychoactive plants and fungi, many of which have been poorly or not studied at all.
We envision the knowledge generated from pursuing research of these natural products will benefit researchers, clinicians, patients and policymakers, and the molecules discovered may give rise to new therapeutic psychedelics with potential for fast-tracking based on evidence from previous human use. The molecular and cellular targets of these identified molecules may also support the development of synthetic drugs with improved properties through traditional pharmaceutical development routes.
Harvard-wide Interdisciplinary Program in Psychedelics
The Harvard Interdisciplinary Program in Psychedelics (HIPP) is a joint effort led by faculty from Massachusetts General Hospital’s Center for Neuroscience of Psychedelics, Dana-Farber Cancer Institute, and Beth Israel Deaconess Medical Center, and provides education on current understandings of clinical, ethical, and scientific dimensions of psychedelic-assisted therapy. This program is accessible to individuals who maintain a clinical appointment with any of the teaching hospitals affiliated with Harvard Medical School.
Our Team
 Jerrold F. Rosenbaum, MD
Jerrold F. Rosenbaum, MD
Director
Psychiatrist-in-Chief Emeritus
Director, Center for Anxiety and Traumatic Stress Disorders
Read full bio
Dr. Rosenbaum, Stanley Cobb Professor of Psychiatry at Harvard Medical School, chaired the Massachusetts General Hospital Psychiatry Department for 20 years, leading 600 clinicians and researchers, and 150 trainees. The Psychiatry Department was ranked by U.S. News and World Report as #1 in the United States in 2019 and for 20 of the prior 24 years, with 60 specialty clinical and research programs and over 70 million dollars in annual research spending. At Mass General, he served as Chair of the Executive Committee on Research.He was the 2007 recipient of the C. Charles Burlingame Award for lifetime achievement in psychiatric research and education and the 2016 recipient of the Joseph B. Martin Dean's Leadership Award for the Advancement of Women Faculty for Harvard Medical School. He is Emeritus Fellow of the American College of Neuropsychopharmacology (ACNP). In 2018, he was an Ellis Island Medal of Honor awardee. He was President/Board Chair of the Anxiety and Depression Association of America (ADAA) and served as President and is a Board member of the American Foundation for Suicide Prevention. He served a six-year term as Trustee of the Massachusetts General Hospital and was Trustee of the Partners Healthcare System. He is co-Chair of Development at Mass General.
He’s co-authored more than 400 original articles and reviews and edited 20 books. He led longitudinal studies of children at risk for anxiety disorders and depression, which examined behavioral differences, risk factors, longitudinal outcomes, treatment, genetics and brain structure and function of children of parents with mood and anxiety disorders.
He is currently the director of the Center for Neuroscience of Psychedelics to understand how psychedelics change the brain and to explore novel mechanisms for treatment of psychiatric disorders. He co-founded Psy Therapeutics to advance the discovery of novel drugs for psychiatric and neurologic disorders and is co-founder of Sensorium Therapeutics, Inc. to explore plant derived molecules as leads for novel psychiatric therapeutics.
Dr. Rosenbaum received his undergraduate degree from Yale College in 1969 and his medical degree from Yale School of Medicine in 1973. He completed his residency and fellowship in Psychiatry at Massachusetts General Hospital, Harvard Medical School.
 Sharmin Ghaznavi, MD, PhD
Sharmin Ghaznavi, MD, PhD
Associate Director & Director of Cognitive Neuroscience
Instructor in Psychiatry, Harvard Medical School
Read full bio
Sharmin Ghaznavi, MD, PhD, is associate director of the Center for the Neuroscience of Psychedelics and the Center’s director of cognitive neuroscience. Dr. Ghaznavi also serves as a psychiatrist at the Dauten Family Center for Bipolar Treatment Innovation and an instructor at Harvard Medical School. Her research interests include the neural correlates of rumination, self-related processing and other cognitive processes underlying mental illness. She has also been leading an initiative within the Department of Psychiatry to research rumination as a transdiagnostic phenomenon.
Dr. Ghaznavi has been the recipient of the Dupont-Warren and Livingston psychiatric research fellowships from Harvard Medical School, as well a 2012 NARSAD Young Investigator Award and a competitive loan repayment award from the National Institutes of Health. Her work has been published in the American Journal of Psychiatry, Biological Psychiatry and Biology of Mood & Anxiety Disorders.
Dr. Ghaznavi received her undergraduate degrees in biology, brain and cognitive sciences, and philosophy from the Massachusetts Institute of Technology. She obtained her medical degree and PhD in neuroscience from Yale University and completed a residency in adult psychiatry at the Mass General/McLean Psychiatry Residency Program. As a resident, Dr. Ghaznavi received the Thomas P. Hackett award for academic and research excellence and the Joyce Tedlow Award from the mood and anxiety disorders board for efforts to integrate psychotherapy, psychopharmacology and research.
 Bruce Rosen, MD, PhD
Bruce Rosen, MD, PhD
Scientific Director, Neuroimaging
Director, Athinoula A. Martinos Center for Biomedical Imaging Professor of Radiology, Harvard Medical School
Read full bio
Bruce R. Rosen, MD, PhD, is director of the Athinoula A. Martinos Center for Biomedical Imaging at Mass General and the Laurence Lamson Robbins Professor of Radiology at Harvard Medical School. He is also the vice chair of research in the Department of Radiology at Mass General.
Dr. Rosen has received numerous awards in recognition of his contributions to biomedical imaging, including the Outstanding Researcher award from the Radiological Society of North America (RSNA) and the Rigshospitalet’s International KFJ Prize from the University of Copenhagen/Rigshospitalet. He is a fellow of the International Society for Magnetic Resonance in Medicine (ISMRM); a Gold Medal winner from ISMRM for his contributions to the field of functional neuroimaging; a fellow of the American Institute for Medical and Biological Engineering and a member of the Institute of Medicine of the National Academies, the American Academy of Arts and Sciences, and the National Academy of Inventors.
Among his many achievements in the biomedical sciences, Dr. Rosen is a pioneer in the field of functional neuroimaging. In the early 1990s, he oversaw development of the technique functional magnetic resonance imaging (fMRI), which measures the hemodynamic and metabolic changes associated with brain activity in both health and disease. More recently, his work has focused on the integration of fMRI data with information from other imaging modalities, including positron emission tomography (PET), magnetoencephalography (MEG) and noninvasive optical imaging. Many of the tools he has introduced are now used by research centers and hospitals around the world to study and evaluate patients with stroke, brain tumors, dementia and neurologic and psychological disorders.
Dr. Rosen received his MD degree from Hahnemann Medical College in Philadelphia, his PhD degree from MIT in 1984 and subsequently completed an internship and residency at Mass General and research fellowships at Mass General and the Harvard-MIT Division of Health Sciences and Technology (HST).
 Stephen J. Haggarty, PhD
Stephen J. Haggarty, PhD
Scientific Director, Chemical Neurobiology
Director, Mass General Chemical Neurobiology Laboratory in the Center for Genomic Medicine
Stuart and Suzanne Steele Research Scholar and Associate Professor of Neurology, Harvard Medical School
Read full bio
Stephen J. Haggarty, PhD is Scientific Director, Chemical Neurobiology at the Center for the Neuroscience of Psychedelics and Director of the Chemical Neurobiology Laboratory within the Center for Genomic Medicine at Mass General. Dr. Haggarty is also Associate Professor of Neurology at Harvard Medical School and has appointments at the Broad Institute and the Harvard Stem Cell Institute. In 2017, Dr. Haggarty was named the Stuart & Suzanne Steele Research Scholar within the Mass General Research Institute.
Dr. Haggarty’s research program operates at the interface of chemical biology and molecular therapeutics with a focus on dissecting the role of neuroplasticity in health and disease. A major emphasis of his work is the use of reprogramming technology to create patient- specific, induced pluripotent stem cells (iPSCs) as powerful new models for the study of neuroplasticity; understanding the neurobiology of human disease; and addressing the challenge of discovering novel targets and next-generation, disease-modifying therapies for brain health using the principles of precision medicine. Dr. Haggarty completed his PhD in the Department of Chemistry and Chemical Biology at Harvard University and post-doctoral training at the Broad Institute.
 Jacob Hooker, PhD
Jacob Hooker, PhD
Director, Translational Biomarkers
Professor of Radiology at Harvard Medical School
Phyllis and Jerome Lyle Rappaport MGH Research Scholar at Mass General
Read full bio
Dr. Hooker is currently Professor of Radiology at Harvard Medical School and Phyllis and Jerome Lyle Rappaport MGH Research Scholar. He received his PhD in Chemistry from the University of California, Berkeley in 2007. Dr. Hooker then completed two fellowships—a Goldhaber Distinguished Fellowship and a Ruth Kirschstein Fellowship—at Brookhaven National Laboratory, where he maintained an appointment as an Associate Scientist through 2013.
In 2009, Dr. Hooker moved to Boston to join the Athinoula A. Martinos Center for Biomedical Imaging at Massachusetts General Hospital. There he co-founded a first-in-class imaging facility that merges functional MRI and positron emission tomography for neurochemical study of the human brain. Dr. Hooker holds associate or affiliate appointments at the Broad Institute, Dana Farber Cancer Institute and the Massachusetts Institute of Technology (MIT). He is an active consultant and advisor to the pharmaceutical industry in neurotherapeutics; he currently serves as a scientific advisory board member for, among others, Psy Therapeutics, Delix Therapeutics, and Fuzionaire Diagnostics. In 2017, he co-founded Eikonizo Therapeutics which leverages molecular imaging to de-risk drug discovery in the pursuit of disease-modifying therapeutics for neurodegenerative diseases. Dr. Hooker serves as Editor-in-Chief of the journal ACS Chemical Neuroscience.
Dr. Hooker’s research program focuses on advancing our understanding of the brain through the development and application of molecular imaging agents. His lab has provided insights into biochemical dysregulation of neurodegenerative diseases and neurodevelopmental and psychiatric disorders in the areas of neuroinflammation, epigenetics and neurochemical dynamics. The program has wide a scope including fundamental radiochemistry methodology, medicinal chemistry, radiotracer development, and preclinical and human magnetic resonance and positron emission tomography imaging. Additional information on Dr. Hooker and his research can be found on the Martinos Center Chemical Neuroscience Program website.
 Franklin King, MD
Franklin King, MD
Director of Education and Therapist Training
Instructor in Psychiatry, Harvard Medical School
Read full bio
Franklin King IV, MD, is the director of training and education at the Mass General Center for the Neuroscience of Psychedelics and a clinical instructor at Harvard Medical School. His primary clinical and research interest is in the utilization of psychedelic-assisted psychotherapy to treat a variety of chronic psychiatric conditions, including depression and anxiety disorders, and in strategies to optimize these interventions for different patient populations. In addition, Dr. King teaches and supervises residents and fellows at Mass General, and practices clinically as a staff psychiatrist at the Center for Anxiety and Traumatic Stress Disorders as well as on the Acute Psychiatry Service in the Emergency Department.
Dr. King received his MD from the University of Massachusetts and completed a residency in psychiatry at Mass General and McLean Hospitals, serving as the chief resident on the Consultation-Liaison Service. Following graduation, he completed a fellowship in Consultation-Liaison Psychiatry as well as a research fellowship with the Mass General Cardiac Psychiatry Research Program.
 Jeremy N. Ruskin, MD
Jeremy N. Ruskin, MD
Professor of Medicine, Harvard Medical School
Founder and Director Emeritus, Telemachus & Irene Demoulas Family Foundation Center for Cardiac Arrhythmias and Cardiac Electrophysiology Fellowship Training Program
Read full bio
Jeremy N. Ruskin, MD is Professor of Medicine at Harvard Medical School and Founder and Director Emeritus of the Telemachus & Irene Demoulas Family Foundation Center for Cardiac Arrhythmias and Cardiac Electrophysiology Training Program at Massachusetts General Hospital. He also holds the Omran Alomran Endowed Chair in Cardiology at MGH.
In 1978, Dr. Ruskin founded the Telemachus & Irene Demoulas Family Foundation Center for Cardiac Arrhythmias and Clinical Electrophysiology Laboratory and the MGH Training Program in Clinical Cardiac Electrophysiology, the first subspecialty clinical service and fellowship program dedicated to the care of patients with cardiac arrhythmias in New England and one of the first in the United States. Since its inception, the MGH Arrhythmia Service has been an international leader in innovative clinical care, research on the mechanisms of and new therapies for cardiac arrhythmias, and the training of future leaders in the field. During his 40-year tenure as Training Program Director, Dr. Ruskin was responsible for the training and mentorship of more than 150 clinical and research fellows in the subspecialty of clinical cardiac electrophysiology, many of whom hold senior leadership positions at academic centers throughout the world. Dr. Ruskin served as a member of the FDA Cardiovascular and Renal Drugs Advisory Committee for 5 years and has worked extensively on the scientific and regulatory aspects of medical device and drug development, as well as the cardiac safety of noncardiac drugs. In 1995, he founded the International Atrial Fibrillation Symposium which he has directed since its inception and is the largest and longest running free-standing meeting on atrial fibrillation worldwide, now entering its 27th year.
Dr. Ruskin’s research interests include mechanisms and prevention of cardiac arrhythmias and sudden cardiac death, brain-heart interactions in patients with atrial fibrillation, new antiarrhythmic drugs and devices for atrial and ventricular arrhythmias, cardiac safety issues in new drug and device development, and new approaches to myocardial preservation using novel biocompatible hydrogels for delivery of drugs and biologics in ischemic injury. He is an author of more than 500 original scientific publications, chapters, reviews, guidelines and monographs. Dr. Ruskin maintains an active regional, national and international referral practice in the field of cardiac arrhythmias and is recognized annually in Best Doctors in America. He is the recipient of the 1997 Michel Mirowski Award for Excellence in Clinical Cardiology and Electrophysiology, the 2002 Heart Rhythm Society Pioneer in Pacing and Electrophysiology Award, the 2015 KCHRS Pioneer in Electrophysiology Award and the 2018 William Silen Lifetime Achievement in Mentoring Award at Harvard Medical School.
In the News
A Long, Strange Trip: Turning Psychedelics into Therapeutics
Sharmin Ghaznavi and Rick Doblin discuss the ethical and legal challenges of proving that psychedelics can be effective and safe medicines on HMS' health policy and bioethics consortium.
Are Psychedelics an Effective Treatment for Mood Disorders?
Jerrold Rosenbaum discusses the potential of using psychedelics, such as MDMA and magic mushrooms, to treat treatment-resistant mood disorders like depression and anxiety on the Ask a Harvard Professor podcast.

Science of Psychedelics for Mental Health Treatment
Dr. Rosenbaum recently appeared on GBH's Greater Boston to discuss the science behind using psychedelics under medical direction to treat mental health conditions.

The Center for the Neuroscience of Psychedelics celebrated their launch headlined by Michael Pollan
Renowned science writer Michael Pollan joined Center leadership to discuss psychedelics research and recent advances in the field of psychedelics.
Can Hallucinogenic Mushrooms Treat Depression?
The Boston Globe recently featured the research of the Center for the Neuroscience of Psychedelics and its work to treat mental health conditions.

The Center for the Neuroscience of Psychedelics was recently featured in The Boston Globe

Jerrold Rosenbaum, MD, talks to WBUR about the new Center for the Neuroscience of Psychedelics
The center will focus on studying how and why the brain reacts to psychedelics, and its research could shed new light on what their use could mean for mental health treatment.

Mass General Launches New Center to Study Psychedelics in Psychiatry
The Center investigates the effects of psychedelics at the molecular, cellular and systems levels across different patient populations.

Arielle’s Legacy Supports Research on Psychedelics
To help others suffering from intractable depression, Arielle’s family created a memorial fund to honor her and advance psychedelic research.

Videos
The Center regularly holds informational salons to shed light on various projects and areas of focus.
The Center for the Neuroscience of Psychedelics: Conversation with Michael Pollan
The Center celebrated their official launch on Tuesday, March 9 with a conversation with Michael Pollan who writes about the places where nature and culture intersect: on our plates, in our farms and gardens and in the built environment. You can download a transcript of the event here.
Psychedelics and Mental Health: Harnessing the Potential for Change to End Suffering
Leaders of the Mass General Center for the Neuroscience of Psychedelics discuss the potential of psychedelics to enhance the brain’s capacity for change and ultimately, transform the care of individuals who suffer from psychiatric illness.
Psychedelics and Mental Health: Neuroimaging the Mind Brain Connection
The Center for the Neuroscience of Psychedelics presents Bruce Rosen, MD, PhD, director of the Athinoula A. Martinos Center for Biomedical Imaging at Mass General and members of his lab, for a deep dive into the power of neuroimaging. Together they describe how cutting-edge tools like PET imaging, Hyperscanning and fMRI will help us understand the ways that psychedelic compounds facilitate lasting changes in mental health and well-being, and how that knowledge will be translated into new therapies and alleviate human suffering.
Watch the video >Psychedelics and Mental Health: Discovering the Therapeutic Potential of Psychoactive Plants
Please join Steve Haggarty, PhD, scientific director of Neurobiology at the Center for the Neuroscience of Psychedelics for a deep dive into the botanical richness and medicinal power of the Amazon rainforest and beyond. In this webinar, Dr. Haggarty describes the planned research of a library of approximately 100 psychoactive plants and fungi, curated by the late Richard Evans Schultes, PhD, Harvard Professor and a founding father of the field of ethnobotany. Dr. Haggarty demonstrates how the knowledge from this research will have the potential to give rise to new therapeutic psychedelics, and how patient-derived and other cellular models can be used innovatively for the discovery of precision medicines targeting neuroplasticity.
Watch the video >Psychedelics and Mental Health: Neuroscience of the Self, Other and Human Connection
Please join Sharmin Ghaznavi, MD, PhD, associate director and director of Cognitive Neuroscience for the Center for the Neuroscience of Psychedelics for a unique look into how psychedelics might be used to facilitate positive, lasting changes in the brain that improve how we understand ourselves and relate to others. Individuals with mood and anxiety disorders tend to see themselves and others in a negative light, resulting in loneliness and poor relationships. By incorporating and leveraging knowledge about which brain regions are implicated in self and other related processing, and how psychedelics facilitate neuroplasticity in these regions, there is immense potential to transform care and reduce, or even, eradicate suffering.
Donate Now
The Center for Neuroscience of Psychedelics has been brought to life by generous donations from our partners.
Department of Psychiatry
For 80 years, Mass General's Psychiatry Department has provided the highest quality patient care through pioneering research.
Over 60 specialty psychiatry clinical and research programs
We provide care for patients of any age throughout the lifespan.
Support Our Work
The Center for the Neuroscience of Psychedelics has been brought to life by generous donations from our partners. Want to help? Email Molly McCarthy, Director of Development, or use the Mass General donation portal and specify that you’d like to designate your gift toward our center.
