Thyroid Nodule Program
Contact Information
Thyroid Nodule Program
Thyroid Associates
Wang Ambulatory Care Center
15 Parkman Street, Suite 730
Boston,
MA
02114
Phone: 617-726-3872 #6
Endocrine Surgery Program
Wang Ambulatory Care Center
55 Fruit Street, Suite 460
Boston, MA 02114
Phone: 617-643-7359
Near Public Transit
Accessible
Explore Our Program
About the Program
The Thyroid Nodule Program is a collaborative program of Massachusetts General Hospital's Thyroid Associates and Endocrine Surgery Program, as well as the Center for Endocrine Tumors within the Mass General Cancer Center. We provide the most advanced diagnostic and therapeutic approaches for thyroid nodules.
Frequently Asked Questions: Thyroid
What is the thyroid gland and what is its function?
The thyroid gland is an important endocrine gland that produces thyroid hormones, which circulate and affect most organs in the body. The major hormones are known as “T4” and “T3”. Thyroid hormone is essential for growth and development, and plays an important role in energy metabolism, and normal cardiac and bone function. When the thyroid is under-functioning (underactive, hypothyroid), patients may feel cold and tired. Although weight gain is typically thought to be a symptom of low thyroid, that is rarely the case. When the thyroid is over-functioning (hyperthyroid, overactive), patients may feel anxious, hot, involuntarily lose weight, note palpitations and rapid heartbeat, and may develop cardiac problems.
The thyroid gland is controlled by the pituitary gland through the hormone TSH (thyroid stimulating hormone). When the thyroid gland is underactive, the TSH concentration is elevated. When the thyroid is overactive, the TSH concentration is low. Measurement of serum TSH is the most sensitive test of thyroid function. A normal serum TSH concentration excludes abnormal thyroid function.
The thyroid gland also produces the hormone calcitonin. The role of calcitonin in normal individuals is uncertain. However, a rare cancer of the thyroid gland (medullary thyroid carcinoma) is associated with elevated serum calcitonin.
The thyroid gland is shaped like a butterfly, with the wings corresponding to the lobes of the thyroid and the connecting piece between the lobes, known as the isthmus. The thyroid gland sits on top of and to the sides of the windpipe (trachea). It sits below the Adam’s apple and above the collar bone. The parathyroid glands , while located adjacent to the thyroid, perform the function of calcium metabolism in the body. The nerves that control the movement of the vocal cords run behind the thyroid.
How can I tell if my thyroid is working properly?
Hypothyroidism (underactive thyroid) may cause fatigue, low energy, muscle aches, cold intolerance (feeling cold, even in a warm room), dry skin and hair loss. When the thyroid is only mildly underactive (subclinical hypothyroidism), patients may or may not be symptomatic.
Hyperthyroidism (overactive thyroid) may cause anxiety, heat intolerance (feeling hot all the time) weight loss despite increased appetite, pounding of the heart (palpitations), difficulty sleeping and shortness of breath. If the thyroid function is only slightly overactive, patients may or may not be symptomatic.
Measurement of serum TSH is the most sensitive test to determine an overactive thyroid. When symptoms suggestive of thyroid gland over-activity or under-activity are present, serum TSH should be measured.
Although many patients have symptoms suggestive of low thyroid, if the serum TSH is within normal limits, it is unlikely that the symptoms are related to the thyroid. If the serum TSH is abnormal, additional blood tests may be necessary. When the serum TSH is elevated, we also measure free T4. When the serum TSH is low, we also measure free T4 and T3.
What kinds of disease affect the thyroid?
Thyroid disease may affect thyroid function, causing hyperthyroidism or hypothyroidism (see above). Thyroid disease may be “structural,” causing enlargement of the thyroid gland (goiter) and/or lumps or nodules in the thyroid. In many cases, a thyroid nodule is discovered incidentally when patients have tests including CT scans, MRI scans or carotid ultrasound examination for other reasons.
In a small number of patients, abnormal thyroid function and structural disease co-exist. For example, some thyroid nodules cause over-activity of the thyroid gland; however, the vast majority of thyroid nodules do not cause abnormalities in thyroid function.
Frequently Asked Questions: Thyroid Nodules & Goiters
What is a thyroid nodule?
A thyroid nodule is the term used for a “lump” in the thyroid. Thyroid nodules are very common occurring in more than 50% of individuals over age 65. Fortunately, about 90% of thyroid nodules are noncancerous (benign). If a physician or a patient feels a lump in the region of the thyroid gland, a thyroid ultrasound will confirm or exclude the presence of a thyroid nodule. When nodules are found incidentally with a CT scan, MRI or carotid ultrasound, a thyroid ultrasound is also indicated to learn as much as possible about the nodules.
Most nodules are asymptomatic. Thyroid nodules rise with swallowing. When large, thyroid nodules may cause a sense of pressure in the neck and rarely may affect breathing and swallowing. Patients with a thyroid nodule should see a physician who can assess and help determine whether a biopsy and/or treatment is needed. A fine needle aspiration (FNA) biopsy may be necessary to determine if a thyroid nodule is benign or cancerous.
What is the difference between a nodule and a goiter?
A goiter is a medical term that means abnormal enlargement of the thyroid. This can appear as a swelling in the front of the neck. One cause of general thyroid enlargement is the benign thyroid inflammation called Hashimoto’s thyroiditis, which may cause thyroid gland under-activity (hypothyroidism). The thyroid gland may also become generally enlarged with an overactive thyroid due to the condition called Graves’ disease. The thyroid may also be enlarged because it contains multiple nodules ("multinodular" thyroid). Multinodular thyroid glands generally function normally, but may be associated with thyroid gland over-activity (hyperthyroidism) in a small portion of cases.
Patients with a multinodular goiter need to have the nodules evaluated by a physician on a regular basis with a physical exam and ultrasound. Occasionally, additional studies such as a CT scan (without contrast) or an MRI are necessary to be certain that the nodules are not causing the airway (trachea) to be narrowed or compressive symptoms such as a sense of pressure in the neck or, in rare cases, difficulty breathing and swallowing.
What causes thyroid nodules to form?
We do not know why thyroid nodules are so common. Although thyroid nodules may run in families, they are so common in the general population that it is often not certain whether the condition is truly genetic. Exposure to excess radiation in childhood increases the risk of thyroid nodules and thyroid cancer (e.g., radiation therapy that was used for acne, scars, enlarged tonsils, and other benign conditions). However, radiation therapy has not been used for these purposes for decades. The benign inflammation known as Hashimoto’s thyroiditis often causes a “lumpy” thyroid, which may be misinterpreted as a multinodular thyroid gland either on physical examination or by ultrasound examination. In areas of iodine deficiency, nodules often grow to large size, but iodine deficiency itself does not cause thyroid nodules.There is plenty of iodine in a typical American diet.
Frequently Asked Questions: Diagnosis & Treatment
How are thyroid nodules diagnosed?
Thyroid nodules are most commonly discovered by chance during imaging studies, such as CT or MRI scans or ultrasounds that are performed for other reasons. Thyroid nodules may be discovered by the patient or a physician during a physical examination.
If you think that you may have a thyroid nodule, you should be evaluated by a physician. You will likely have the following during your evaluation:
- Physical exam with a review of your medical history
- Blood test to check the function of your thyroid (i.e. thyroid stimulating hormone (TSH) test). If thyroid function is overactive (low TSH), a radioactive iodine scan may be performed
- Thyroid ultrasound to verify the presence of the nodule, assess the size and characteristics (fluid-filled or solid) and assess for other nodules in or around the thyroid
- Depending on the findings, a fine-needle aspiration biopsy may be recommended to check the kinds of cells in the nodule and to ensure they are benign (noncancerous)
Many patients just want to know if their nodule is a sign of thyroid cancer. Your physician will use information from your history, physical exam, blood work and biopsy results to determine if a particular nodule requires a biopsy or treatment.
What are the treatment options for thyroid nodules that are shown to be non-cancerous (benign) on FNA biopsy?
For patients with normal thyroid function and thyroid nodules, observation with periodic physical examinations and ultrasounds are necessary to be certain that the nodule is not changing. Repeat biopsies may become necessary if the nodule size or ultrasound characteristics change.
When thyroid nodules cause local symptoms, exhibit continued growth or are a source of anxiety, surgery is often the appropriate treatment option (see patient videos).
When thyroid function is high (hyperthyroidism) in a patient with thyroid nodules, radioactive iodine or surgery are both excellent alternatives. In some patients, medication alone is used to control the thyroid over-activity.
What are the treatment options for thyroid nodules that are shown to be cancerous (malignant)?
Nodules that are suspicious on biopsy are usually treated with surgery. Treatment for most cancerous thyroid nodules begins with surgery, although some very small, slow growing tumors may be observed bases on recent data. The most common thyroid cancers are called well-differentiated thyroid cancer and include papillary thyroid carcinoma, follicular thyroid carcinoma and Hürthle cell carcinoma. After surgery for well-differentiated thyroid cancer, radioactive iodine therapy may be necessary to destroy remaining thyroid tissue or treat residual cancer in more advanced cases. Learn more about thyroid surgery.
Medullary thyroid carcinoma also requires surgery, but there are special considerations. In some patients, this cancer is associated with an adrenal tumor called a pheochromocytoma, and that must be excluded prior to thyroid surgery. In some patients, this cancer runs in families, therefore patients may require specific genetic testing. Patients benefit from a multidisciplinary team with expertise in endocrine oncology.
What are the treatment options for nodules that are considered "indeterminate"?
Approximately 20-25% of FNA biopsies of the thyroid are considered indeterminate. This means that we cannot definitely decide whether the nodule is benign or malignant based on that biopsy alone. Several alternatives are available for indeterminate biopsies depending upon the specific biopsy result. These include:
- Repeating the biopsy
- Repeating the biopsy with special tests to analyze the genetic make-up of the tumor
- Considering surgery for a definitive answer
When should I see a doctor?
It is important to see a doctor if you think you may have a thyroid nodule or goiter, or if you are experiencing abnormal swelling or pressure in your neck, especially with difficulty breathing or swallowing. You should also see a doctor if you experience any of the symptoms of hypothyroidism or hyperthyroidism over an extended period of time.
What is the Thyroid Nodule Program at Mass General, and how do I make an appointment with a specialist?
The Thyroid Nodule Program is a collaborative program of Mass General’s Thyroid Associates, Endocrine Surgery Program, as well as the Center for Endocrine Tumors within the Mass General Cancer Center. Specialists with different areas of expertise collaborate closely in the Thyroid Nodule Program and offer a complete and multidisciplinary evaluation to patients with suspected or diagnosed thyroid nodules. Appropriate diagnostic studies and treatment options are recommended based on their findings.
Appointments are available at Thyroid Associates at Mass General in Boston, Newton-Wellesley Hospital, Mass General - Waltham, and at the Mass General/North Shore Center for Outpatient Care in Danvers.
Patient Resources
These videos and slides can help to answer your questions about thyroid treatments and anatomy.
Sareh Parangi, MD, endocrine surgeon in the Thyroid Nodule Program at Massachusetts General Hospital, discusses thyroid nodule biopsy results and treatment recommendations for patients.
Roy Phitayakorn, MD, endocrine surgeon, and Giuseppe Barbesino, MD, endocrinologist, of the Thyroid Nodule Program at Massachusetts General Hospital discuss patient outcomes and ongoing care after thyroid surgery.
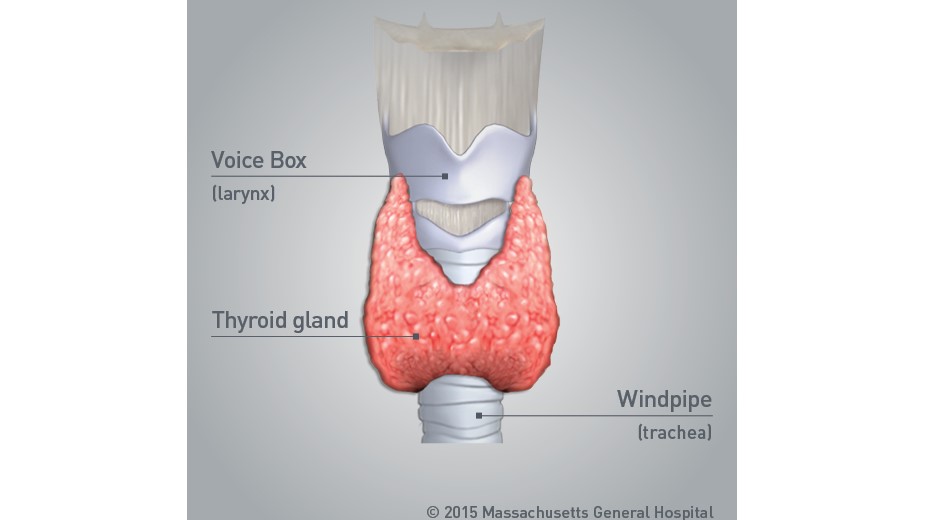
The anatomy of a healthy thyroid gland
Our Surgeons
We bring together a team of experts in the management of patients with both benign and malignant thyroid, parathyroid and adrenal conditions.
-
![]()
- Section Head, Endocrine Surgery Program
- Associate Professor of Surgery, Harvard Medical School
- Attending Surgeon, Mass General Brigham Healthcare Center (Danvers)
-
![]()
- Thyroid, Parathyroid, and Adrenal Surgeon
- Co-Director, MGH Thyroid RFA Program and NWH Thyroid Biopsy Clinic
- Quality Chair, MGH Department of Surgery
-
![]()
- Chief, Division of Gastrointestinal and Oncologic Surgery
-
![]()
- Clinical Affiliate, Mass General
- Lecturer on Surgery, part-time, Harvard Medical School
-
![]()
- Chair of Surgery at Newton-Wellesley Hospital
- Director MGH Thyroid Cancer Research Laboratory
-
![]()
- Associate Surgeon, MGH
- Associate Professor of Surgery, Harvard Medical School
-
![]()
- Massachusetts Eye and Ear Director, General and Thyroid/Parathyroid Endocrine Surgical Divisions
- Harvard Medical School Professor of Otolaryngology Head and Neck Surgery
- Claire and John Bertucci Endowed Chair in Thyroid Surgical Oncology
-
![]()
- Director of Mass General Endocrine Surgery Fellowship
#1 Research Hospital in America
Mass General is recognized as a top hospital on the U.S. News Best Hospitals Honor Roll for 2023-2024.
Contact Us
Specialists from the Thyroid Nodule Program answer frequently asked questions about thyroid nodules and goiters and refer patients for appropriate studies, treatment, and follow-up when needed.








