Genes Expressed in the Brain Before Birth May Affect Risk of Childhood Mental Illness
Study’s findings provide additional evidence that risk for mental illness in children begins in the womb.
Contact Information
1 Bowdoin Square, 7th Floor
Boston,
MA
02114
Phone: 617-643-6010
Fax: 617-643-6060
Email: leap@partners.org
The Learning and Emotional Assessment Program (LEAP) at Massachusetts General Hospital provides neuropsychological evaluations to children and adolescents, ages 2 to 22. We specialize in the assessment of neurodevelopmental and psychiatric disorders, learning disabilities, attention deficit hyperactivity disorder (ADHD), autism spectrum disorder (ASD), anxiety, and mood disorders. Many children also have neurological or genetic conditions (e.g., seizures, tics, etc.).
Our evaluations provide a comprehensive and in-depth perspective on a child’s cognitive (thinking), emotional, behavioral, and social functioning, integrating information from parents, teachers, and standardized testing. We rely on our deep knowledge of child development and neuroscience to identify a child’s strengths and weaknesses. We aim to clearly communicate conceptualizations to parents and providers, and make practical recommendations about needed treatment and school supports. We are committed to providing culturally sensitive evaluations.
Please note that LEAP currently only accepts referrals for new patients from within the MGB system. MGB Providers should submit referrals via Epic referral order REF13228 AMB REFERRAL TO MGH PEDIATRIC NEUROPSYCHOLOGY. Established families who have been seen at LEAP in the past can request re-evaluation by calling our office at 617-643-6010, option 2.
LEAP is located at 1 Bowdoin Square, 7th Floor, Boston, MA 02114.
LEAP Address: 1 Bowdoin Square, 7th Floor, Boston MA 02114
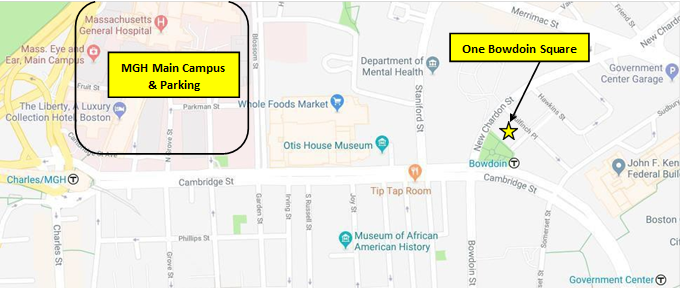
1 Bowdoin Square is located on the corner of Cambridge Street and New Chardon Street, approximately 0.5 miles from the Mass General Hospital’s Main Campus.
There is no parking at our building. We recommend parking in the MGH main campus garages, where you will pay the patient rate. It takes approximately 15 minutes to walk to our building from MGH. There is also a free shuttle service between the MGH main campus and Bowdoin, which the Information Desk inside the main hospital can call for you (please allow 20-25 minutes for shuttle arrival). Please note that parking fees at nearby commercial garages vary vastly in prices, and we cannot validate for these parking expenses.
Our building is accessible via public transportation. There are several nearby MBTA stations:

LEAP evaluations are a collaborative process that actively engages the patient, their family, and the referring clinician.
Gretchen L. Timmel, M.Ed., Educational Specialist, Learning & Emotional Assessment Program (LEAP)
Areas of Expertise:
A: The first step is for your child’s MGB provider to place a referral to our clinic via Epic (order number REF13228). Please note that due to high demand, as of November 5th, 2022, LEAP is only accepting new patient referrals from providers within the Mass General Brigham, or MGB Healthcare System. We are currently unable to accept referrals for new patients who do not have an MGB provider. If you are an established family with LEAP requesting a re-evaluation, we will accept a self-referral even if your child does not have an MGB provider. Please let us know (via phone or email) if this is your situation and we will provide further information about how to place a referral. Please note that referrals are needed for all evaluations, even if you have been seen at LEAP in the past.
Once we receive a referral, our insurance team will determine if prior authorization is required by the child’s primary insurance. Please ensure that your child’s insurance information is up to date in their MGH medical record. To update your information, please call Patient Registration at 866-211-6588.
We schedule in the order in which we receive referrals, and we will reach out to you to schedule your appointment as soon as possible. Please be advised that due to high referral volume, patients over 4 years old should expect to receive a scheduling call from our clinic approximately 11 months from the date of referral. The wait time for children under 4 years old is shorter. Please ensure that your contact information is up to date in the child’s MGH medical record. To update your information, please call Patient Registration at 866-211-6588.
A. For young children, you might tell them that they are going to meet with a doctor to do some activities like the ones they do at school so the doctor can figure out how they learn best. For adolescents, you might tell them that they are going to meet with a doctor to do a variety of tests that will help the doctor to figure out how they learn best. It may be helpful to tell your child that they can’t study for these tests and that they aren’t expected to get everything right – they are only expected to try their best.
Research is an important component of the Learning and Emotional Assessment Program's (LEAP) mission. Each clinical evaluation yields valuable information, which patient can choose to share to help further LEAP's mission. These data can be used to answer scientific questions that have implications for the patients we see and are always privacy protected to ensure anonymity.
The cornerstone of LEAP's research initiative, led by Alysa Doyle, PhD, is the Longitudinal Study of Genetic Influences on Cognition (LOGIC). This project has allowed us to build a permanent but flexible research infrastructure at LEAP, including a database to organize our enormous repository of information and a mechanism that allows patients to contribute to research.
Through this study, patients allow us to use information collected from their assessments. Patients can also fill out additional questionnaires and provide DNA for genetic analyses. The fluidity between the clinical and research realms that LOGIC represents resulted in this project winning the 2014 hospital-wide Clinical Research Day Team Award at Massachusetts General Hospital.
To date, LOGIC has collected data from over 1,000 children and adolescents. We have used this information to publish papers and garner grants from various foundations and the National Institutes of Health. The questions we are interested in answering include:
This research infrastructure has also allowed us to develop collaborations across the hospital, including:
Our team aims to grow the baseline sample of LOGIC to data from 3,000 youth. A data set of this size with information about genetics, neuropsychology, learning and emotional problems will allow us to answer the questions above and learn more about conditions like autism spectrum disorder, ADHD, mood disorders, anxiety disorders and psychosis.
We also aim to launch the longitudinal follow-up of the LOGIC study. In this arm of the project, we will meet with youth enrolled in the study over time. This follow-up will allow us to learn more about why some children do well while others continue to struggle. Understanding different trajectories should also create new opportunities for early identification of those at risk.
Finally, we are using our database to train a new generation of clinical researchers. The fellows who rotate through LEAP can develop or contribute to research projects relevant to the LEAP population. Papers currently under development include understanding sensory processing and social difficulties across a range of conditions.
Depending on funding, full-time research assistant positions are often available for those who have completed undergraduate studies. Please direct any questions to Dr. Alysa Doyle, LEAP’s Research Director, at doylea@helix.mgh.harvard.edu
We are grateful for the funding that has allowed us to grow our research program. We are particularly indebted to the Stanley Center for Psychiatric Research at the Broad Institute of Harvard and MIT for their ongoing support, as well as to the David Judah Foundation for helping us to launch our research program and to the National Institutes of Health (NIH).
Our clinical professionals have devoted their training, research, and clinical practice to acquiring the specialized skills needed to assess children with learning disabilities, psychological disorders, and developmental disorders.
Molly Colvin, PhD, ABPP, Director; Co-Director, Child Psychology Internship
Ellen Braaten, PhD, Executive Director
Alysa Doyle, PhD, Director of Research
Michael Capawana, PhD, Director of Psychometric Training
Cara Cordeaux, PhD, Co-Director of Postdoctoral Training
Gina Forchelli, PhD, NCSP, Co-Director of Postdoctoral Training
Madeline Manning, PhD
Gretchen Timmel, MEd, Educational Specialist
Chardā Davis, PsyD
Emily Peters, PhD
Marissa Roth, PhD
Heidi Sarles-Whittlesy, PhD
Alyssa Sullivan, PhD, PAC/LEAP Lifespan Fellow
Regan Summers, PsyD
Elise Taverna, PhD
Megan Henley
Tabinda Khan
Shannon Mulcahy
Rachel Spencer
Molly Witt
Sarah Mancuso, Group Practice Administrator
Abigail Ross, Patient Services Coordinator
Our 2-year postdoctoral fellowship in pediatric neuropsychology focuses on clinical training in the consultation, assessment, and provision of feedback to parents, referring physicians, and schools of children and adolescents (2–22 years). Fellows have opportunities to participate in ongoing research projects with current staff and provide tiered training and supervision to clinical interns and psychometrists. Training experiences and didactics are tailored to conform with ABCN and Houston Conference/Division 40 training requirements to support eventual board certification in clinical neuropsychology with an emphasis in pediatric neuropsychology.
Positions are typically announced in the early fall, with an application deadline in early December. Applicants should have a doctoral degree from an APA/CPA-approved program in psychology, preferably in Clinical Psychology, although applicants from other programs will be accepted. Successful applicants will have prior experience in assessment and working with children/adolescents. Completion of the doctoral degree and an APA/CPA-approved predoctoral internship are required before the fellowship start date. Fellows hold clinical appointments in the MGH Department of Psychiatry and academic appointments in the Harvard Medical School.
For additional information, please contact training directors Dr. Gina Forchelli (gforchelli@mgh.harvard.edu) and/or Dr. Cara Cordeaux (ccordeaux@mgh.harvard.edu).
LEAP is a primary training site for the Child Psychology Track of the APA-accredited MGH predoctoral internship. Interns spend approximately half of their time engaged in evaluation services at LEAP. The Child Psychology seminar is also coordinated by LEAP. Please direct any questions to Dr. Molly Colvin, Co-Director of the Child Psychology Internship at mcolvin@mgh.harvard.edu.
We are pleased to announce immediate openings for full-time pediatric clinical neuropsychologists.
View the Pediatric Clinical Neuropsychologist job description
If you would like to support the work of the LEAP program, please contact the Development Office.
For 80 years, Mass General's Psychiatry Department has provided the highest quality patient care through pioneering research.
The Division of Child & Adolescent Psychiatry at Mass General for Children provides comprehensive psychiatric services for children and teens.
We provide care for patients of any age throughout the lifespan.
Study’s findings provide additional evidence that risk for mental illness in children begins in the womb.
Like the rings of a tree, teeth contain growth lines that may reveal clues about childhood experiences.
The death of a family pet can trigger a sense of grief in children that is profound and prolonged, and can potentially lead to subsequent mental health issues.
Suicide is a scary subject to talk about for many families. If you know what to look for, suicide is often preventable.
It can be difficult or even scary to learn that your teen is harming him/herself. This handout will talk about different types of self-harm and signs of possible self-harm. It will also give you tips on how to help your teen if he/she is self-harming.
In this Q&A, learn more about how depression affects children and how you can help your child from Mai Uchida, MD, director of Early Identification and Prevention of Pediatric Depression and provider in Child and Adolescent Psychiatry at Mass General for Children (MGfC).
The integration of patient care and clinical research has been a hallmark of the Department of Psychiatry for more than 30 years. Today, the department has the largest clinical research program in the hospital, with studies at the forefront of neuroscience, molecular biology and genetics.